Why pituitary tumours cause visual problems
You have two optic nerves – one behind each eye. Optic nerves act like cable wires that send information from your eyes to your brain. This allows you to see. These two optic nerves meet and partially cross over at the base of your brain at an area called the optic chiasm.
The pituitary gland sits very close to the optic nerves and optic chiasm, just behind your eyes.
Because of this, a pituitary tumour (pituitary adenoma) can touch or press on these nerves, often at the chiasm. When this happens, the nerves can no longer send visual information properly, which can lead to eyesight problems.
If you have a larger tumour (also called a macroadenoma), you have a higher risk of developing vision problems. This is because the tumour is more likely to press on your optic nerves and optic chiasm.
What eye problems can you have with a pituitary tumour?
Blurred vision: This is when objects you see look unclear or out of focus.
Double vision: This is when you see two images of a single object at the same time.
Reduced peripheral vision: This is when you find it hard to see anything that is not directly in front of you.

You may find out you have a pituitary tumour after an eye test. This can happen when you notice changes to your vision and get your eyes tested, or after a routine eye test. You may then be told that you have lost part of your vision, which is called visual field loss. This could lead to you having further tests done such as an MRI scan which may find that you have a pituitary tumour.
It can be scary to be told you have a pituitary tumour after what may have been a routine eye exam. If you are diagnosed with a pituitary tumour, it's important to know these are often benign (non-cancerous) and that treatment is available.
Finding out you have eyesight problems after getting diagnosed with a pituitary tumour
Your endocrine doctor will likely arrange for you to have an eye examination after you are diagnosed with a pituitary tumour, particularly if the tumour is close to or touching the optic chiasm.
After you are diagnosed with a pituitary tumour, it is important that you have an eye examination, especially if you have problems with your eyesight. This is because an eye examination can look for eye issues which may be caused by your pituitary tumour.
If you are having problems with your sight and have not had an eye exam, you should speak to your GP or endocrinologist about this.
What to expect at your eye exam
Below are some of the tests you may have:
Visual field test
Peripheral vision is how well you can see objects you are not directly looking at, outside of your central vision. If your pituitary tumour is pressing on your optic nerves, this can affect your peripheral vision.
A visual field test is used to measure your peripheral vision and can help to monitor your pituitary tumour. During this test, you will be asked to look straight ahead and press a button every time you see a flash of light appear.
Visual acuity test
This test is used to measure how well you can see at a specific distance.
During this test, you will be shown a chart with letters of different sizes. You will be asked to read the letters out loud.
OCT scans (also known as Optical Coherence Tomography)
This scan shows detailed images of the back of your eye, including the optic nerves. It can be used to check if the tumour is putting pressure on them and can also be used to monitor for any signs of change.
During this test, you will be asked to rest your chin on a machine. The machine will then take a scan of your eye, which should take a few minutes. The machine will not touch your eye and this scan is completely painless.
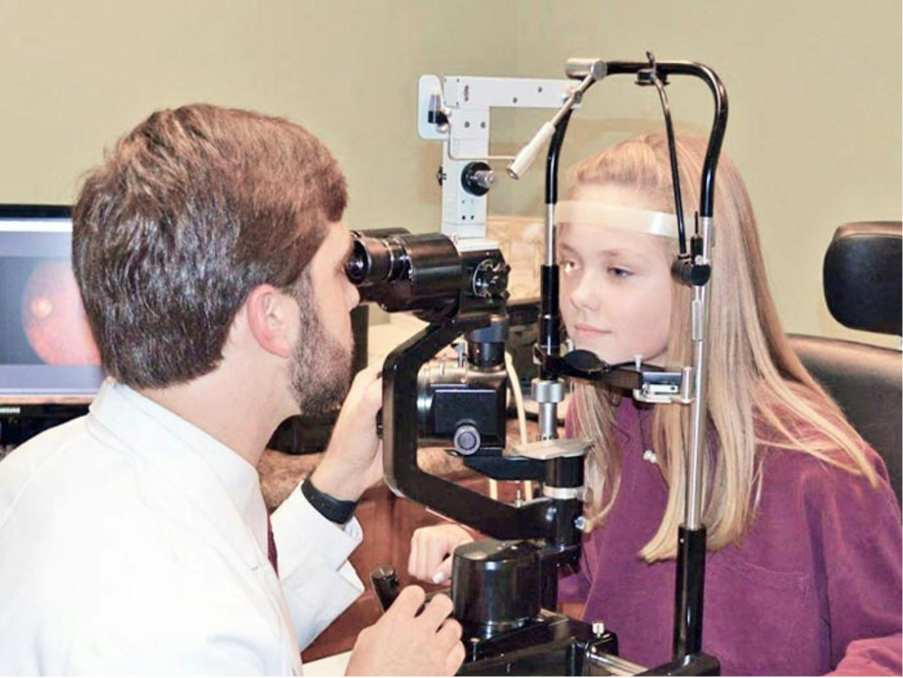
Monitoring your eyesight after a pituitary tumour diagnosis
After you are diagnosed with a pituitary tumour, you need to get your eyes tested regularly. This is often every 6 to 12 months but your healthcare team should advise you on how often you should have an eye exam.
If you notice any changes to your vision, it is important to contact your eye specialist or medical team.
Driving restrictions
The Driver and Vehicle Licensing Agency (DVLA) handles driving licenses in the UK.
The DVLA needs to know about any condition you have for over 3 months that could impact your ability to drive. This means that if you have a pituitary tumour, you need to tell the DVLA.
Many people with a pituitary condition can drive, but you need to check with your GP. If your condition causes eyesight problems you may have driving restrictions.
You can also find more information on driving with a pituitary condition.
How to look after your vision after pituitary tumour surgery
Before your surgery
You may have surgery to remove your pituitary tumour. Before your surgery you may be seen by a member of the ophthalmology team. This is usually done when the pituitary tumour is in contact with the optic nerves.
After your surgery
After surgery you will need to stay in hospital for a few days. Before you are discharged from the hospital, you may be asked if you have any problems with your vision. This will often happen if you had problems with your eyesight before your surgery.
If the tumour was pressing on your optic nerves, your vision may improve after surgery. This can sometimes happen quite quickly. People who had mild or recent vision problems often notice the most improvement.
If your vision problems were severe or long-standing, you may still have some ongoing issues even after treatment.
Who might you see in an eye clinic?
Ophthalmologist: A medical doctor that diagnoses and treats eye problems.
Ophthalmic technician: A healthcare professional that helps the ophthalmologist by carrying out tests such as visual fields and OCT imaging.
Specialist orthoptist: A healthcare professional who can diagnose and treat problems with your eye movements. They can also diagnose and treat problems with your binocular vision. This means how well your eyes work together. Orthoptists may work in pituitary clinics as part of your care team.
Who you see about your eyesight will depend on which hospital your care is under and what services they have in place. You may be directed to see your local optician for your usual routine eye test if there is a lower risk of eye problems. Please speak to your endocrinologist to find out what is necessary in your care and who may carry out your eye test.
About Rareminds
Rareminds is a UK-based charity supporting the mental health of those with rare diseases and their family members. They provide access to specialist counsellors and psychotherapists trained in working with rare diseases.
They have a unique understanding of the psychosocial impact of rare diseases and work in partnership with patient organisations, rare disease charities and groups to understand the specific challenges faced by their communities.
All of their counsellors/psychotherapists have additional post-Diploma (or equivalent) level experience, and have completed Rareminds internal training programme on ‘Counselling for those impacted by Rare Diseases’.
We are currently offering two services with Rareminds. The first is a 1-1 counselling service. The second is a group therapy programme. Please note you cannot sign-up for both the small group programme and 1-1 support.
Meet the counsellors
Dr Stephanie Yin, Psychotherapist (UKCP), Psychologist (CPsychol)

Stephanie is an accredited psychotherapist and counsellor, and a full clinical member of UKCP. She has worked with children and adults in NHS and community counselling services for several years. Informed by both a lived and professional experience, she is passionate about raising awareness and improving mental health services for the rare disease community.
Stephanie also conducts research and provides training and consultancy on the experience of living with rare and chronic conditions.
Stephanie is the lead counsellor, but depending on capacity you may be seen by another member of the Rareminds counselling team.
Sign-up for 1-1 support
This service offers members up to 8 sessions of free, confidential counselling service. This will be on zoom, or on the phone, and is available for family members and individuals aged 18+ impacted by a pituitary condition.
Both evening and daytime appointments are available (weekdays only).
As living with a pituitary condition happens within the context of your everyday life, it’s inevitable that the ‘ups and downs’ of both impact on each other. You can talk to our counsellors about anything that you are struggling with in living with the emotional impact of a pituitary condition.
This service is only open to enhanced members of The Pituitary Foundation. You can become a member for £25 a year, and there are concessions available.
You will also need to purchase our enhanced membership package of £15. This brings the total cost to £40 to access the service. With our enhanced membership offering you get access to the 8 counselling sessions and an informative video to help with your wellbeing.
Once you have purchased the enhanced membership then you will be sent information via email on how to arrange an initial consultation with our lead counsellor, Stephanie. Once you have emailed, you should expect a response within 5 working days. Please note that there may be a waiting list, and your initial consultation or sessions may not begin for a few weeks depending on current capacity. We encourage you to make contact after purchasing your membership, even if you don’t intend to start sessions straight away.
We have limited funding for our counselling service so places are offered on a first come, first serve basis. We are aware that the demand for this service is very high and we aim to manage the demand the best that we can. We anticipate that demand will be high so it is likely that we will have to close the service soon after the reopening, but we can reopen as places become available. In our experience, demand evens out after an initial influx so hopefully we won’t have to close and reopen too often.
Sign-up for small group sessions
Please read all the information below before signing-up for the group.
This service is open to everyone in our community, and you do not need to be a member of The Pituitary Foundation to sign-up. The Spring 2026 group sessions will be limited to people who have been newly diagnosed with a pituitary condition for less than two years.
This new small group programme will involve a combination of information and group discussion on themes such as living with uncertainty, making the most of appointments, coping with family and relationship dynamics, and managing anxiety.
It will provide a supportive, confidential space to share experiences and meet with others experiencing similar situations. Over the 8 weeks there is an opportunity to explore common themes, discuss practical and emotional coping strategies - and meet online with others in a similar situation. Bring a big cup of tea or coffee too!
The sessions will run weekly on a Monday from 7.00pm to 8.30pm (Zoom). The first session will be Monday 2nd March 2026. There will be a maximum of 12 programme participants and, although we understand ‘life happens’, please be prepared to commit to the full 8 week programme in principle. Places will be allocated on a first come first served basis, as spaced are limited.
The waiting list for this group is now full.
On the morning of Sunday 12th February 2023, I woke up with a splitting headache, vomited and when I looked in the mirror both of my eyes were full of blood. On the Monday, after much badgering from my wife and mother, I called the doctor. My GP wanted to check for a mini-stroke and so I went to A&E at my very small local hospital. The A&E doctor did a CT and asked why my legs and hands were so swollen, I explained that’s just how I am and that I sleep with flight socks on to help but the swelling always comes back the next day. About 30 minutes later he said they had ‘found a Mass’.
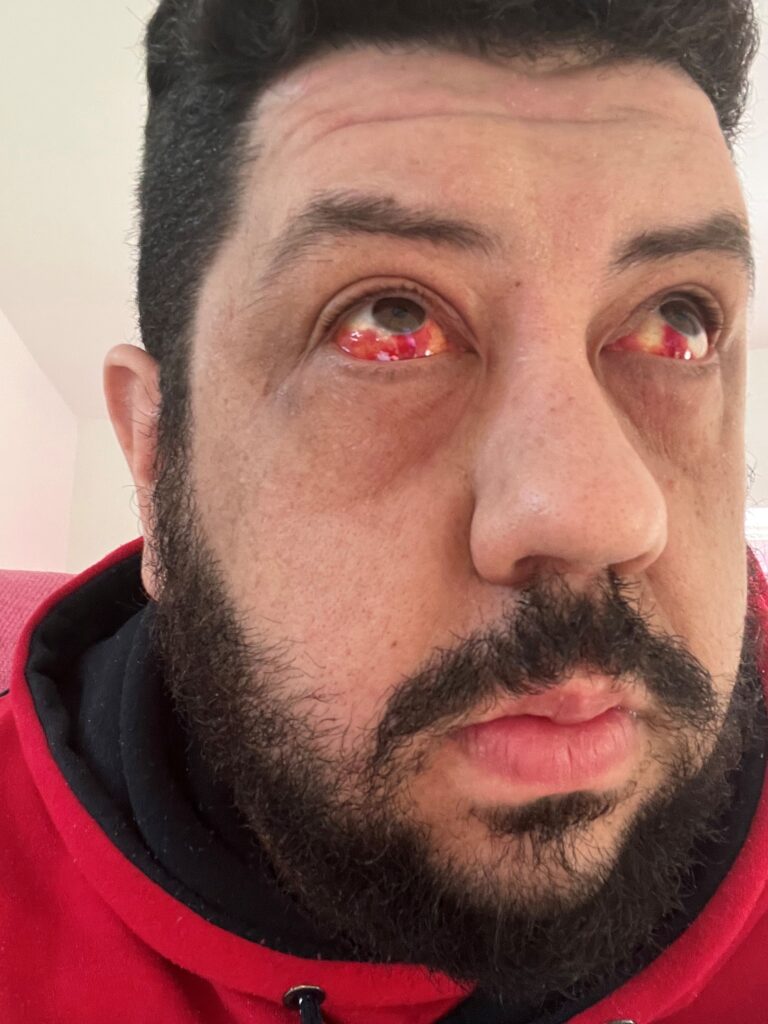
I remember being terrified, they wouldn’t discharge me until the nearest major hospital said it was ok to do so and they were talking about blue-lighting me over to there. As far as I knew in that moment, I was dying.
My wife and I had known for years that there was something not quite right; I had been swelling for a long time. On holiday in 2011 we noticed that one side of my chest was larger than the other. When we got home I went straight to the doctors who ran some bloods and found I had low testosterone and raised prolactin. I was referred to the local hospital where the specialist was completely uninterested and sent me away to lose weight.
For years after that we just got on with it until my symptoms really ramped up during the first Covid lockdown. I have a very sedentary, office-based job. I think during a particularly busy time my phone logged a total of 168 steps in 1 day. When I started to gain weight and my ankles and feet were swelling we simply put it down to that. I tried to move more, my wife would push me out of the front door for a walk, but I was still swelling, I put on about 35kgs of weight in a few months. It got to a point where my legs would hurt because the skin was so tight. So, again, I went off to the GP and explained the situation and again, they told me to lose weight.
Once the CT was done, life changed. It was decided I had a Pituitary macroadenoma and over the next few months I had what felt like every test the NHS knew how to do: Nuclear scans, MRI’s, CT’s, blood tests, OGTT’s. The list goes on, but eventually it was decided the tumour had given me Acromegaly. The normal range of IGF-1 for my age is 14.9 -32.4, mine at that time was 131.2.

Acromegaly is awful and because it’s rare it doesn’t get talked about that often. As well as the swelling it gives you horrendous joint pain, you sweat uncontrollably even when it’s cold, it can affect your organs, my lower left jaw moved to what felt like a 45-degree angle and I couldn’t close my mouth properly. I was referred to QMC in Nottingham and was prescribed Octreotide in a very small dose. I felt excellent for the first week, it was life changing, but then my body felt like the batteries had been taken out. After harassing the endocrine nurse, it was agreed that they would increase the dosage and begin monthly Lanreotide LAR. Before I had the nuclear scan, I had to come off the Octreotide for 3 days and I could barely walk.
After some issues with my treatment in Nottingham I asked to be transferred to Addenbrookes, which is where I ended up having my operation. The Endocrine and Neuro team at Addenbrookes are really very good, I felt safe despite the fact that Acromegaly makes surgery very hard, it had given me sleep apnoea as well which the anaesthesiologist wasn’t happy about and my weight was a real problem. But the surgery was a success, I had a CSF leak which caused me to be very ill, but otherwise it went well.
It turned out my tumour was a triple hormone secreting adenoma; Prolactin, TSH and Growth hormone. It was pushing on my pituitary and almost completely preventing testosterone production. My endocrinologist called whilst I was writing this and she tells me I’m now confirmed to be in remission from Acromegaly, my IGF-1 is now 29. The acromegaly will never go completely, but I’m in the best position I have been in for a long time.
My wife was my hero through the whole episode, she was a rock and I have to say the biggest thank you to her, she kept me alive just as much as the hospital did.
After ready Amy’s story- a 10 hour operation, I felt inspired to share my own story, which started off very similar.
In 2022 4 weeks after a violent altercation, I awoke with a severe headache. Having abstained from alcohol since the January of 2022, I had drunk a glass of wine the previous evening and put the headache down to dehydration. Unfortunately, the headache did not subside and by 09:00 hrs I had to ask my wife to call an ambulance. Paramedics were quickly on scene (fortunately) tests for stroke carried out and then a swift trip to our local hospital. The 12 hours wait in the car park in the back of the ambulance was broken with first a cat scan and then a full MRI.
The result was that my tumour had burst and was showing signs of compromising my optic nerves. A field of vision examination revealed that my vision was impaired in both upper left and upper right quadrant, indicating pressure on the centre of both optic nerves.
I had a trans-sphenoidal re-section of the tumour, and fortunately the whole of the tumour was removed. Following 7 days in hospital I am fortunate that I was allowed home and my only residual symptoms are low levels of 2 hormones and slightly impaired taste and smell.
Recently I had an appointment with my endocrinologist. My review went well and I am pleased that my blood levels have stabilised and the consultant informed me that they will continue with annual blood tests and MRI scans for this year and then review gain after my next annual review.
The consultant has given me photos of my pituitary scans, before and after surgery.
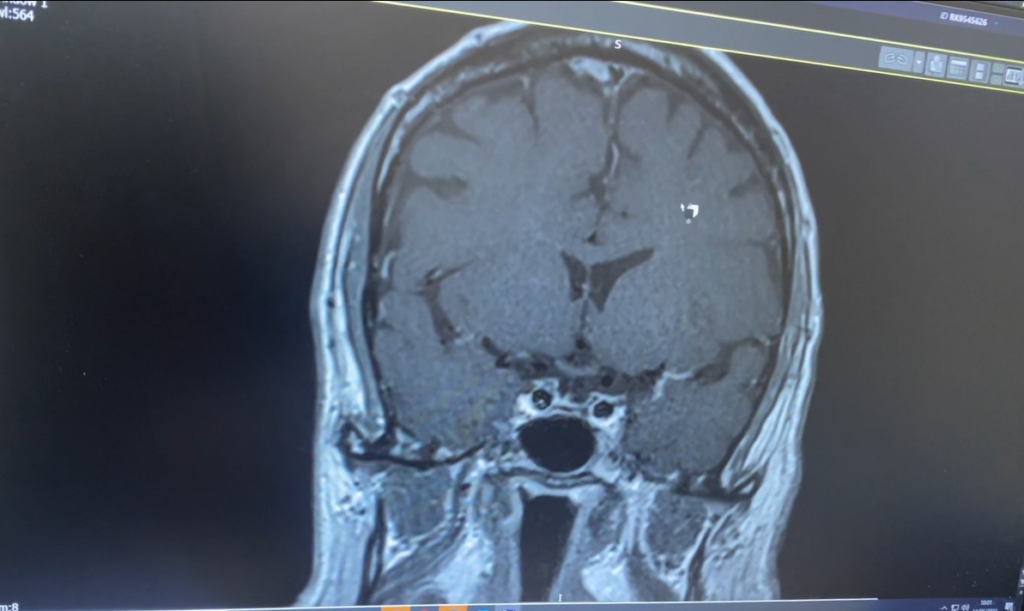
Reading Amy’s story really does make me feel so fortunate and indicates how narrow the margins for success and failure really are. I wish her well for the rest of her treatment and hope she has a successful session of radiotherapy and that they can rid her of the rest of the tumour.
The foundation is an awesome thing as I have taken comfort myself from stories that have been covered. I hope that my story can be of similar comfort to others.
My name is Jhori Morris, and I would like to share my prolactinoma (Pituitary Adenoma) journey in hopes that it may help someone else who may be experiencing some of the things I experienced.
I stopped taking oral contraceptives around November of 2022, and that’s when some of the symptoms started to arise, but I didn’t think too much of it, as stopping contraceptives may cause issues initially hormonally.
My journey of diagnosis/potential treatment started last year around April/May of 2023. I noticed a significant amount of weight gain, despite trying to lose weight. I also experienced amenorrhea, which is the absence of menstruation, galactorrhea, and absence of ovulation. After my physician ordered lab work, the results at the time seemed to be consistent with PCOS (Polycystic Ovarian Syndrome). After failed rounds of fertility medication, my doctor referred me to a Reproductive Endocrinologist. After the work up with the Reproductive Endocrinologist, I found out everything anatomically was normal, and there were no tubal or uterine issues other than small fibroids. My Reproductive Endocrinologist proceeded with additional lab testing, which included thyroid studies, and Insulin Resistance testing. The lab results indicated that I was Insulin Resistant, and had hypothyroidism.
My symptoms/fertility issues continued, and in February of this year, my Reproductive Endocrinologist ordered a MRI of the brain, and that’s when I was diagnosed with a pituitary adenoma. Thankfully, my tumor was not large enough to indicate surgical removal! Since, I have started or oral medication to help with hypothyroidism, weekly injections to aid with the Insulin Resistance. I have also started an oral medication twice weekly, called Cabergoline, a dopamine promoter, which treats high levels of prolactin in your blood.
As my journey has just begun, I’m noticing improvement with weight, and blood prolactin levels are trending downward.
I hope my store can help someone else! I have a great team of health care providers that were swift with testing and diagnosing, and have shown so much support during this time. Always be an advocate for yourself, and make sure you and your provider find the best treatment options appropriate for your situation.
My name is Risa and I have Acromegaly.
It was October of 2018, as I nervously awaited the results of my brain MRI. I remember utter disbelief washing over me as my Endocrinologist informed me that I had a large tumour on my Pituitary Gland and furthermore, it was causing a rare disease with a name I couldn’t even pronounce.

Seven years earlier, I began noticing changes in my body and overall health. I was an extremely active endurance athlete; Ironman races, long distance cycling, CrossFit and anything outdoors were my fun. But I soon started experiencing extreme weight gain, an inability to recover after workouts, changes in eating habits, severe headaches, to name only a few. I discussed these and the other symptoms with my Primary Care Physician time and time again, pleading for some insight and hoping for solutions. I didn’t feel heard, it was as if the doctor didn’t believe me.
In 2018, I was at my wit’s end, and after three attempts of requesting (the final request was more like a demand) a brain MRI, the tumour was discovered. My symptoms had advanced so much by that point, that it became difficult for me to leave my home. Along with this diagnosis came some relief and validation, I finally had an explanation for all the symptoms I was experiencing for so many years. It wasn’t in my head. I wasn’t making it up. I wasn’t crazy! Then it hit me, in that very moment I knew going forward I must use my voice, speak up, and trust that I know myself better than anyone! I became my own advocate and an advocate for others. Doctors don’t always like me now; I am very vocal about my needs and desire to discuss all options.
I spent the year of 2019 recovering from brain surgery, enduring six weeks of radiation treatments, and making excessive trips to the doctor’s office for testing and lab work which continues to this day. I have been left with complications from surgery and I am still working with my Endocrinologist to get my hormone levels under control and find a medication that works for me. This can take a toll on my body, mind, and spirit and requires grace through my process of letting go of my old self.

Looking ahead, my life looks different. I am no longer the person I used to be and have grieved for her. My future is uncertain. My healing continues through the work I do personally and in my Gestalt practice. In my efforts to move forward, I am doing what I can to spread awareness around rare Pituitary diseases/disorders.

I built my strength and confidence back up and rode my bike the 1,845 miles (2969.26 km) from Canada to Mexico down the Pacific Coast (USA) and went on to write an award-winning and 5-star awarded memoir about my bike ride, diagnosis, and personal life upheaval. I have been interviewed on over 30 podcasts to date and give inspirational talks on resilience. My next journey in May 2024 will be along the Camino de Santiago in Spain. Most importantly however, I have become a better human, I have more gratitude and I am creating the best life I possibly can…a life unleashed.
You can find me at www.risaaugust.com

This story has been nearly thirty years in the making. The timing never quite felt right as I always had hope that better things were to come. Fortunately, this optimism has paid off and I have recognized what was holding me back from starting writing.
My pituitary story started in the spring of 1995, when I was 14. I first remember struggling with two things: reading became a problem, with the tops and tails of the characters becoming indistinguishable, meaning d, g, a and q all looked the same; and my colour vision deteriorated. This progressed over a few months with my vision deteriorating further with permanent “floaters”, like when you look at a bright light and best described as black holes in my vision. Over the months these became both more numerous and bigger, meaning I was down to around 30% vision.
The optician noticed issues with the blood vessels at the back of my eyes and referred me to the GP for a diabetes test, which was negative. I was then referred to a community ophthalmologist, who told my mother I was attention seeking and not to pander to me! Luckily, he did refer me to a specialist at Moorfield’s Eye Hospital, and I was fortunate enough to be looked after by Mr Riordan-Eva, who pretty much diagnosed me immediately. He was amazing, spending his entire morning clinic with me, listening to my symptoms, running tests, taking bloods and arranging follow up tests, the first of which was a CT scan.
The other tests proved unnecessary. The CT scan showed a craniopharyngioma and I was immediately introduced to Mr Hayward, who was now my consultant paediatric neurosurgeon. The next five days were a whirlwind, with an MRI scan scheduled to assist with surgery and admission to Great Ormond Street Hospital for a craniotomy.
Looking back in hindsight there were other obvious symptoms too. The debilitating headaches (put down to migraine), slowed growth (a late developer) and frequent passing of urine being some others.

The surgery went better than expected and afterwards I didn’t even realise I had come out of surgery. Except there was one thing that was different. What was it? I couldn’t quite pin it down. Then three days later I realised, with the words that will live with me forever: “Mum, I can see! I can read the nurse’s name badge. Susan Joyce, Staff Nurse”. The relief is impossible to put into words!
This pre-internet-era-naivety was both a blessing and a curse! I think it was natural to think “right, well that’s done, I was lucky, phew, onwards and upwards”. Sadly, that was not to be. A nasty chest infection in hospital was the first rude awakening, setting me back in my recovery. Then there was the small matter of my entire pituitary gland being removed in the operation. Can’t be that important can it?

Turns out the little pea sized gland behind your eyes is vital! Learning new terms and medicine names was overwhelming at first (thank you to The Pituitary Foundation for being by side throughout!), but soon becomes second nature and I now consider myself a patient expert. I am on the full set of replacement meds: hydrocortisone, desmopressin, thyroxine, growth hormone, testosterone and vitamin D.
I am able to say I have been very lucky! Despite a year of building up my strength and attending school perhaps ten times for an hour or two at a time in the first year of my GCSEs, I was able to catchup and get great results, moved on to A levels and got a degree in Economics at University College London (next door to my Consultant Endocrinologist, which was handy!).
It wasn’t all plain sailing however. Stopping growth hormone, aged 19, in the first year of my degree left me bedridden and I nearly failed the first year of my degree as I could barely make it to my exams. Luckily with support from my Endocrinologist I was soon back on the GH and back on track and graduated with a first class honours. Since then I have qualified as an accountant and work full-time in Finance.
There have been ups and downs since. Often it takes a while to adjust to changes in my medications and doses. Things have fortunately come a long way in the time I have been a patient. No more having to carry a cool bag with me everywhere I go and worrying about how my DDAVP will absorb as I have yet another blocked nose from taking a nasal spray three or four times a day!
However, the biggest progress has by far been in the psychological space. At the time of my treatment in 1995 there was precious little support in this regard. I went through the years afterwards feeling generally lucky to be where I was (the waiting room in GOSH is a great place to get perspective!). I couldn’t really understand why over time I felt increasingly numb and like I had lost my spark.
Then 22 years after my operation I had the breakthrough (unfortunately via a breakdown). To cut a long story short, diagnoses and treatment for depression, anxiety, perfectionism, low self-esteem and low assertiveness amongst others led to the underlying cause. I had PTSD.
That made so much sense and after several years of on and off treatment I am now in a far better place. My brain is continuing to readjust after so many years of living in fight or flight mode, and I am now feeling ready and able to share my story.
I remain optimistic about the future and it is so positive to see new developments being researched, after what has felt like a long period of stability. The two projects I am personally most excited about are the effects of oxytocin replacement and the patches to monitor cortisol levels throughout the day. I’m sure both will benefit me and many other patients in future.
My top tips are definitely keeping a sense of humour and finding your passion. For me I realise music is really important and is a good insight into how I am feeling, which allows me to respond in a positive way. Also be your own advocate when you feel you are not being listened to by doctors. It is great to know The Pituitary Foundation is also there for us when we need them.

What is psychological support?
Maintaining good mental wellbeing while living with a pituitary condition can be challenging. As well as supporting you with the clinical side of navigating a pituitary condition, we’re also here to support your mental and emotional wellbeing. This psychological wellbeing hub houses all our psychological support offerings. Here you’ll find publications, articles and videos designed to help you understand and support your own psychological wellbeing.
We have also partnered with Rareminds to provide individual counselling, or group therapy sessions, for anyone diagnosed with a pituitary condition. You can find more information on this below.
Video Resources
Below you will find recordings from previous events aimed at supporting your mental wellbeing and providing practical tips to help you.
Looking after your emotional wellbeing
Body positivity and confidence
Publications Library
Longer Reads
Browse our longer reads to find content related to you

Rareminds support
Find out more about our Rareminds counselling service, including what we offer and how you can access this
RaremindsUpcoming events
Are you struggling with the social and emotional impact of visible difference?
FaceIT@Home is a free, evidence-based online programme designed to help you manage appearance-related anxiety, build confidence, and handle everyday social situations more comfortably.
Read more
Rareminds wellbeing hub
Resources and information from Rareminds, to help you live as well as possible with your rare condition.
Read more
Looking for something to listen to?
Tune in to the Rareminds podcast for information on the go
Listen now
In Summer 2019, Edy noticed that everything was very dark. “It felt like I was wearing sunglasses, all the time. Whether I was inside, outside, raining, sunny, everything was very dark. And I remember being outside and lifting my glasses, thinking they were sunglasses, because everything was dim.” That’s when she realised something was wrong.
She also realised that she couldn’t recognise anyone’s faces in the school she worked in. After visiting an ophthalmologist, she was advised to see a neurologist. During this time, Edy was unable to work, read or drive. Whilst waiting for the appointment she had to go to the emergency room where she was diagnosed with a non-functioning adenoma. It was three centimetres in diameter and pushing on her optic nerve.
Edy had little support from her regular doctor: “My primary care doctor was no help. We ran the typical labs and she said everything looks normal. I had gained a lot of weight, and I was losing my hair, and she said, ‘you need to take better care of yourself. You need to exercise more and get better sleep.’ There was no help at all.”
After her diagnosis, Edy, although supported by her friends and family, felt like no one really understood what she was going through. “They didn't really understand what was going on or how it was affecting me. I was at home and learning about it myself, so I was able to educate others as I learned. They became more supportive with time, but no one knew what this was.”

After her diagnosis Edy had surgery to remove the tumour. Unfortunately, the neurosurgeon was unable to remove any of the tumour as they “didn’t have the proper tools,” since they hadn’t realised how fibrous the tumour was. Unfortunately, the surgery had a huge impact on Edy “I woke up from that surgery, so nauseous, and vomiting all the blood in my stomach, and she tells me that we have to go in again. And I'm just like, no!”
Edy had her second surgery 8 weeks after the first, this time with the correct tools and two surgeons. “Due to the location with the carotid artery and the time constraints, they were only able to get two thirds of the tumour out. So when I came out of that, it was a 20 hour surgery. My poor husband. I went into surgery at eight in the morning, and I wasn't moved out of the operating room until after midnight.” As they weren’t able to remove the entire tumour Edy was told that she could either have surgery again or have six weeks of radiation.

Edy had radiation which was able to shrink the tumour, and it hasn’t grown since. Unfortunately, more recently Edy experienced a spontaneous cerebral spinal fluid (CSF) leak, and had to have a third surgery. She is now on hormone replacement for cortisol and hypothyroidism. “My vision and my optic nerve are permanently damaged because the tumour had been sitting against it for so long. But it is what it is. I can read, I can write, I can drive. It's functional, although it's definitely not perfect.”
The entire experience changed Edy’s outlook on life. “Prior to the tumour I was working nine to five, five days a week. Juggling work and home and kids and family, and it was exhausting. Then this happened and my life was in flux. When my vision returned, and I could see the colours of the flowers outside, it was amazing. Every sunset was fascinating. I couldn't believe how lucky I was to be seeing those amazing colours again!”
During Edy’s recovery, she journaled her experiences: “After the second surgery, my radiation was delayed because of COVID, and I needed to process what I was going through. I decided to start writing it down in a journal.”

Edy ended up writing this journal into a book. “I wanted to write something that could be shared with family or friends of patients going through this. Or even the doctors to help them understand it from the patient’s perspective. They're often desensitised to what it does to a person, so I wanted to write something that would give perspective, from the physical standpoint, the emotional standpoint and how it affects the family. I ended up writing this novel about my experience. I'm so proud of it. I think it's helped a lot of people. I just wanted to provide a layer of support, because I feel like a lot of times people don't get it, especially the mood and the hormonal aspect. I know everyone is different, but I truly believe that the emotional journey we all go through is very similar.”
You can read Edy’s book, The havoc in My Head, on amazon.


















