Anyone who has a rare medical condition will tell you, there's no rule book to 'living well.' Living well can mean different things for different people, and what 'living well' means after a rare diagnosis, may be very different to what it meant before. We know pituitary conditions can drastically change many areas of life. If you've been diagnosed with a pituitary condition and are struggling with the changes this brings, we're here for you. Our resources and support services can help you live well with a pituitary condition, whatever this may mean for you.
Whilst everyone's experiences with pituitary conditions are different, it can be helpful to learn from each other and our shared experiences. To celebrate Rare Disease Day 2026, we held a patient panel event and heard from three members of our Lived Experience Committee, David, Aleha, and Roz. Our patient panel shared their tips for how they live well with a pituitary condition.
The session started with the panel giving a background to their conditions and involvement in The Pituitary Foundation. The speakers have over 50 years of collective experience living with pituitary conditions!
Challenges our panel face
During this part of the talk, the panel each discussed the biggest challenges they have faced in living with a pituitary condition.
Accepting a lack of control
One panel member explained that their biggest challenge is the lack of control they feel over their condition, energy levels, and general health. Days of feeling significantly less well are unpredictable and can be frustrating to live with. To help manage this, they’ve identified and implemented parts of the day where they can take complete control. For them, this means having a deliberately slow and peaceful morning, to prioritise self-care and find a calm start to the day.
If lack of control is something you struggle with, you may want to carve out times in your day when you can find a sense of control. This could be taking an hour for yourself over lunch, to read or go for a quiet walk. Alternatively, you may like to dedicate time to watching a favourite show or movie in the evening.

Recognising and responding to emergency situations
For another panel member, who lives with adrenal insufficiency, the main struggle has been understanding the significance of adrenal crisis and accepting when the situation is an emergency. Their personality has been to play down the situation, which has often made the crisis worse. In order to address this, they’ve made sure the people around them (their partner/family/friends) are aware of the severity of adrenal crisis, and are prepared to support them. This is important to remember when going on trips – are you travelling with people who will recognise a crisis and help you administer an injection?
If you struggle to recognise the signs of adrenal crisis, our information on adrenal crisis and sick day rules can help. Our Adrenal Insufficiency Action Plan is also a great resource to tell others about your condition, what medication you need and what to do if you have an adrenal crisis.

Download our Adrenal Insufficiency Action Plan
Download our Action Plan for free, or order a printed version to be posted to you.
This action plan is a useful resource for anyone with adrenal insufficiency or Addison’s disease, to record essential medical info and share with others to make them aware of your condition.
Download for free or orderCompounding challenges
For the final panel member, who lives with acromegaly, the biggest challenge has been the multifaceted nature of pituitary conditions; it is often one thing after another and so on. With acromegaly, it’s common to also have issues with joints and fatigue. These additional challenges can be hard to deal with, and can get in the way of daily life. Being involved in different areas of the pituitary community, via forums and attending events, and meeting others who can relate, has been helpful with this.
If you are finding it difficult to manage all the different challenges your condition may bring, speaking to others who understand can really help. The Pituitary Foundation runs online and in-person support groups, educational events and regional get-togethers, to bring together people from the UK who are affected by pituitary conditions. You can find out more and get involved through our events page.
Fatigue

Fatigue is a very common symptom experienced by people living with pituitary conditions. Both pituitary conditions themselves and their treatment can cause fatigue. For some, it’s a symptom they struggle with every day, and for others, it’s something that comes out of the blue every few weeks. It can be really tricky to find out what may be causing fatigue for you, but there are things you can try that may help.
All of our panel members reported experiencing fatigue. To help manage this, our panel talked about recognising when the fatigue is overwhelming, and planning around this. Can you move back any commitments to in a few days’ time, where they’ll be more manageable? In order to do this, you need to accept the situation and scale of fatigue, which is a challenge in itself. Trying to communicate the fatigue with family members, colleagues, and friends will help people around you set their expectations of what you can do.
Tips from our event attendees:
- Using the ‘spoon theory’ can be a really effective way to talk about fatigue with people who don’t have lived experience of fatigue
- One attendee has breakfast in bed every morning in order to give her first dose of hydrocortisone time to kick in
- Another attendee has got into the routine of getting up early in the morning to make a coffee for their partner, and wanting to provide this act of service motivates them to get up on harder days
Pituitary surgery
Surgery as an experience can be challenging for different reasons. For routine and planned operations, the process is generally well-planned, and the procedure will be explained clearly. During this event, the panel talked about emergency surgery, which can be more stressful. In these situations, signing a consent form while feeling very unwell can be a scary experience.
Post-surgery, there can be lots of unexpected outcomes. One panel member discussed feeling really emotional and waking up in the night crying, unsure why. This lasted for a few weeks after surgery and was a shock to the system.
Surgery can also make you feel extremely fatigued, which is normal. You should expect to not be able to return to your normal activities for at least a few weeks, if not longer, after surgery. It's also important to remember that everyone's experiences of surgery and recovery are different, and there is no set rule for how long it takes to recover. Being gentle and kind to yourself during recovery is important, as your body has been through something significant. You can find more information on surgery here.
Managing lots of medications for pituitary conditions
Our panel members take a variety of medications, which can be complex to manage. Some medications are simpler, as they can be taken first thing in the morning, or last thing before bed. Other medications are tricky as they happen in the middle of the day, when you might be out and about.
To help with remembering to take these, one speaker recommended using alarms (via a phone/watch/bracelet). They also recommend having a follow up alarm 15 minutes later, in case you miss the first one!
Another speaker associated different medications with different aspects of her daily routine. As they take a bus home at the same time every day, they have built the rhythm of taking a medicine while on the bus home.
It’s also important to confirm what medicines need to taken with food, and which needs to be taken on an empty stomach. To confirm this, the speakers recommend speaking to an endocrine nurse about the various medications you’re taking and getting a plan together for each one.
If you are taking multiple hormone replacement medications, it is also important to know if they interact with each other, and how. You can read more about this here.
Tips from our event attendees:
- One attendee recommends keeping medications in a small plastic bag, so if any blister packs fall out, you’ll be able to find them
- Another attendee has a folder ready which explains their different prescriptions and medications, in case they are taken into hospital and needs to explain this to a health care professional

Travelling with a pituitary condition
Travel can be a complex process for people with pituitary conditions. For one of our panel members, the main issue arises around moving between different time zones, and how this affects the timings for their medications. Our panellist finds it helpful to speak to an endocrine nurse or endocrine team to put together a clear timetable for when to take medications while abroad, and to transition doses into the new time zone. Our Nurse Endocrine Helpline can help you with this.
Another top tip is to be conscious of where your medication is while travelling. If you are putting a bag in the hold of an aeroplane or a baggage rack on a train, it might be more sensible to keep your medications in your hand luggage, in case your other bag goes missing. It can also be helpful to take double quantities of your medication, and pack these in separate bags/pockets.
Tips from our event attendees:
- Your endocrine team will be able to write a letter explaining what medications you take for you to show airport security. This will also be able to explain any specific requirements for the medication, for example, that it needs an ice pack while on a flight.
- Lots of airlines and train companies internationally recognise the hidden disability sunflower lanyards. These can help staff be aware you may need extra support at stations or airports or might need a seat rather than standing in a queue.
- One attendee recently travelled with work, and found it really helpful to have a conversation with their colleagues about their condition, so they could feel more prepared in case something went wrong.
- Another attendee always checks where the nearest hospital is to their accommodation is when travelling.
Returning home from hospital stays
After being discharged from hospital, it can be difficult to adjust when returning home. When you're in the hospital, medications will be administered by IV, and oral doses will be managed by the team caring for you. When you return home, you will need to manage your medications yourself. This can take a while for you to feel familiar with. You may find that your other routines, like eating and sleeping, are out of sync while you adjust to new medication routines.
Our panel noted that it is important to acknowledge how difficult this can be. There can be lots of changes to adjust to after coming home from hospital, and it may take time to feel normal again. For our panel member, it was helpful to have a support network in place who could help throughout the adjustment process.
If you are able to, having your support network ready to help you can make a big difference at times like this. Asking friends, family and neighbours to help out with food, laundry and driving you to and from the hospital, can all make a big difference. Being specific with what help you may need can make it easier for loved ones to support you.
Tips from our event attendees:
- Your endocrine team will be able to provide you with instructions for returning home after a hospital stay, which will include a dosing plan when swapping from IV to oral steroids.
FAQs from our attendees
How can you manage mixing the powder and liquid vials in an adrenal crisis?
Your local endocrine team will be able to provide steroid education, but you may need to ask for this. You can also ask that carers/relatives/family members are given this training too. If you live alone, do you have a neighbour who might be able to assist in a crisis?
It can feel scary to think of having to mix powdered hydrocortisone in an adrenal crisis, but the best thing you can do is prepare yourself with the knowledge of how to do it, and when. Watch our video on this, to know what to do.
Since the move away from red-flagging, it’s important to register your address as a high-priority with your local ambulance service. You can find out more about this here. Ambulances carry hydrocortisone kits, which will be administered in a crisis.
What should you be aware of when travelling with pituitary apoplexy? Are headaches a normal symptom?
Yes, headaches are experienced by lots of people with pituitary apoplexy. While travelling, it’s important to think about timeframes, with most NHS trusts suggesting waiting 6 weeks before travelling. It’s important to speak to your own endocrine team before flying, and confirm this is safe to do, and that enough time has passed.
Do you have any tips to manage pituitary conditions and weight gain?
This is a common issue, and you should speak to your endocrinologist about the options available. You could consider a diet that is high in protein and fibre, which helps you feel fuller for longer. Steroids can cause your blood sugar to spike, so looking at reducing sugar intake when taking hydrocortisone is important.
It’s also helpful to keep a record of your weight, and share this with your endocrine team, so they can be aware of any trends or significant changes.
Exercise can be helpful for lots of people here. One panellist started a sport to stay motivated and tries to maintain an exercise routine in her day-to-day life.
Tips from the chat:
- If you don’t have the energy to leave the house for exercise, would an at home walking pad be an option instead?
- For those with AI, timing your exercise around hydrocortisone dosing can help with energy levels. For example, planning a gym trip for 30 mins after an afternoon dose
Read more about pituitary conditions and weight management here.
October is Pituitary Awareness Month and this year, the theme “A Lifetime of Hormone Health” feels especially meaningful to me. Living with a pituitary condition has shaped my life in ways that are often invisible to others, but it has also shown me the importance of resilience, self-advocacy, and hope.

At 19, I was told by a gynaecologist that I would never have children. No clear explanation was given, just a life-changing statement that left me bewildered. Despite this, I went on to have fertility treatment and I’m now blessed with two amazing grown-up children, aged 24 and 22. At the same time, I lived with a constant and frightening thirst, drinking litres of water every day and running to the toilet every 15 minutes (sometimes less). I thought my kidneys were failing. Doctors only tested my blood sugar and reassured me I didn’t have diabetes, but that was of little comfort. What was really happening was vasopressin deficiency, a rare condition that is still poorly understood today.
Growing up, my body didn’t develop in the way it should. I developed just one breast, never started periods like other girls my age, and even had surgery to check whether I had a womb because my uterine lining was so thin it didn’t show up on scans. People often comment on my height (I am 4ft 10”) but few realise how closely this is tied to my pituitary function.

You hear a lot about the challenges of menopause these days. For me, the exhaustion and hormone depletion that many women experience later in life were already there throughout my 20s, 30s, and 40s. I would put on a bright, energetic face in public, only to collapse in private, needing to rest. Even when I tried to explain, one friend scoffed that I was “hardly a geriatric.” This is what makes pituitary conditions so hard; they are invisible illnesses. People don’t see the constant struggle.
"I would put on a bright, energetic face in public, only to collapse in private, needing to rest."
The hidden impacts showed up in other ways too, for example, needing steroids that were missed for years, having a bone age of 70 when I was only 32, and the daily uncertainty of a pituitary gland that only partially functions and seems to “behave” on its own terms.
But I refused to give up. I worked relentlessly in the gym, not just to look my best, but to fight for my bone health and overall wellbeing. Over time, the difference has been extraordinary. At 54, I feel healthier than ever thanks to persistence, better treatment, and greater awareness of pituitary conditions.

And here’s the wonderful part ... life continues to surprise me. Against all odds, I’ve just been signed by a wonderful inclusive modelling agency, ZBD Talent!
In Eleanor Mills’ words, there is still “Much More to Come!”
#ZBD #Zebedee #InclusionRevolution #PocketRocket #PituitaryFoundation
My story starts in 2020. I had headaches, dizziness, was constantly tired and generally rubbish. I had an MRI and they found a tumour; I had a pituitary macroadenoma. The very thought of a tumour was alarming and it was in Covid times, therefore I wasn't able to see anyone for support. A month previous, I found out I was pregnant and as you can imagine, I was filled with dread and so many questions.

I was told by my employer that due to my illness they could not carry on my employment- another whack in the face! My whole life as I knew it was uncertain. I was scared and felt alone. I also suffer from depression and anxiety and this was through the roof. I tried to maintain a positive mentality for my twelve year old daughter; it was hard.
I was told that I needed surgery however, due to the pregnancy, this could not happen until after I gave birth. I was also told that it was a rarity to get pregnant whilst having this diagnosis. As such, a case study has been written. I had regular scans and, towards the end of the pregnancy, the tumour was getting larger. Apparently this can happen due to the pregnancy hormones. The symptoms were getting worse and my sight was deteriorating. The surgeon said they could not wait any longer and I was booked in to have a caesarian section five weeks early. I was informed that I would be unable to breast feed as this would also increase the tumour. I felt a failure. I wanted to give birth to my son naturally and feed him. My mental health was crashing.
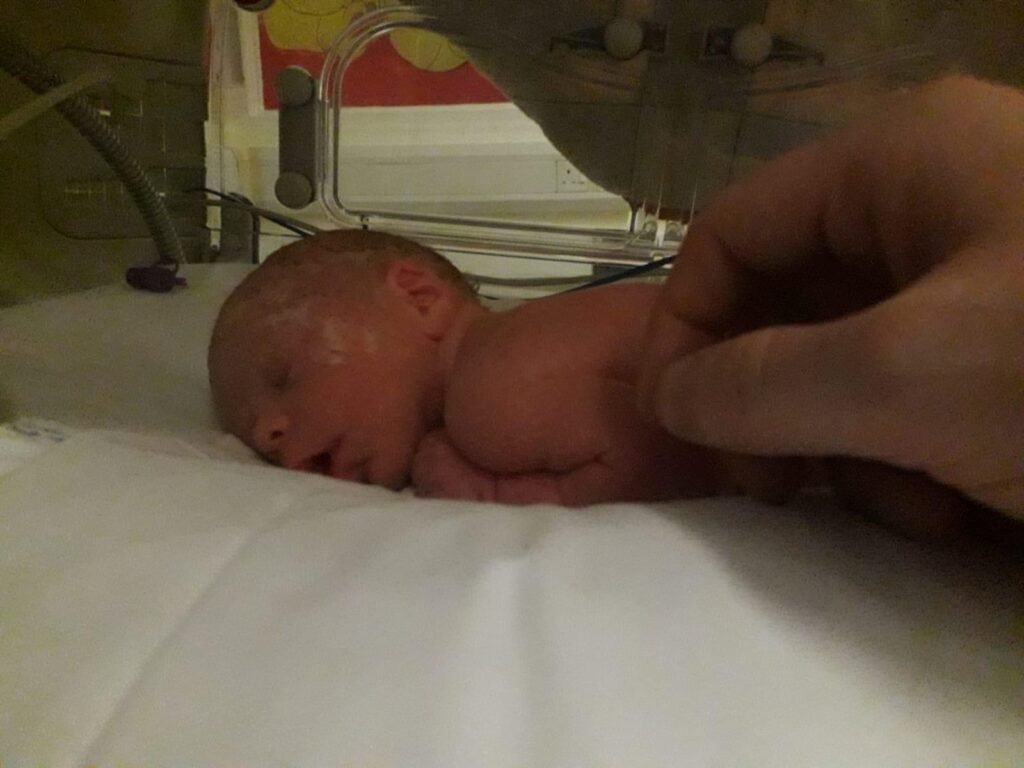
I was informed that I would be unable to feed him as this would also increase the tumour. I felt a failure. I wanted to give birth to my son naturally and feed him.
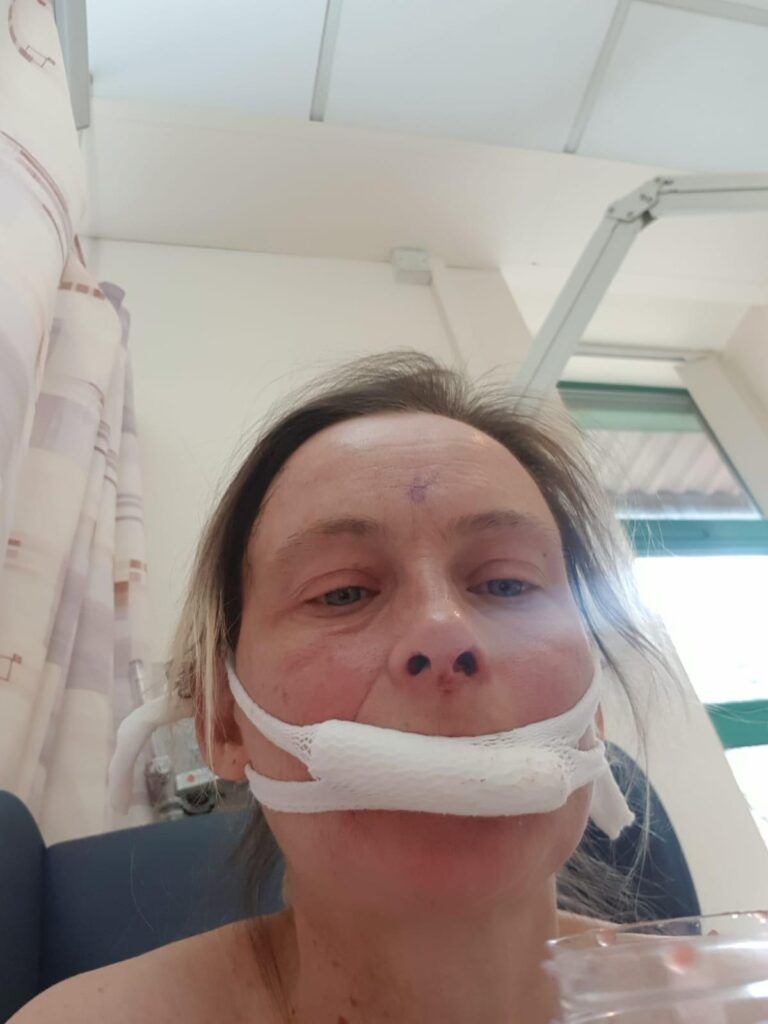
Within two weeks of giving birth to my son, I was in a special neurological hospital having the tumour resected. I could not have asked for better treatment and reassurance. Due to Covid, I was unable to see my partner or children. I came out of hospital six days later and it was a long recovery because of the caesarean, brain surgery and depression.
I have not worked since. I am still constantly tired. If I have a productive day, the next day I am wiped out. This would make it hard going into a job as I couldn't be reliable. This upsets me, as I am skilled and proficient as a financial trader and market manager.



Life is not the same. I have no sense of smell or taste, however if I ask myself how grateful am I? The answer is easy. I look at my children, I breathe in the cold air, watch the birds flying, I am beyond thankful I am here.
Prefer to watch instead of read?
This information is also available as a video! Click on the button below to watch now.
Watch the video!Significant or major life events will happen or touch all of us in some way at some point. Indeed, being diagnosed with a pituitary condition would count as a major life event for most people. Unfortunately, having a pituitary condition doesn’t exempt you from, or inoculate you against, experiencing other kinds of major or key life events. For example, it’s vanishingly unlikely that you’ll never experience a bereavement, and while some people do live in the same house all their lives, most of us don’t, and so we must face the upheaval of moving.
I think major life events are significantly stressful for several reasons, some of which I’ve outlined here. For instance, they can happen unexpectedly (for example, a car accident or a loved one having a stroke) and we mostly have to deal with them alongside the other stuff we’ve already got going on in our lives. If I had to pick a key defining characteristic that marks significant or major life events from daily hassles, it would be that such significant things happen to us only rarely. They are less familiar to us, and we are therefore less practised at dealing with them. That unfamiliarity adds to our stress, general distress and anxiety and can lead us to feel a little (or a lot) lost and uncertain.
Additionally, life events can be overstimulating by exposing us to lots of unfamiliar people, places and things to do. With overstimulation can come overwhelm and problems sleeping, which can be the case even if the event is something we have chosen to do and are looking forward to (such as leaving home, or getting a new job). Research suggests that several key life events happening together in one year in the life of someone who is healthy can be enough to see them developing an illness because of the stress. Which would suggest that significant life events are things that have the potential to cause serious problems for people with long term health conditions such as pituitary conditions.
Learning as a coping strategy
As adults, others expect us, and we expect ourselves, to know how to do things. But why should that be the case for things that don’t happen all that often? We can put a lot of pressure on ourselves and make the stress worse if we don’t acknowledge that our experience of some things is very limited because we don’t do them all that often. Giving yourself permission to approach things with something of a beginner’s mind can be very helpful in reducing some of the stress. As Helen Macdonald puts it in H is for Hawk...
‘Being a novice is safe. When you are learning how to do something, you do not have to worry about whether or not you are good at it. But when you have done something, have learned how to do it, you are not safe any more. Being an expert opens you up to judgement.’
Telling others that you haven’t done this for a while, or indeed ever, can be useful in eliciting sympathy, advice and support.
Coping with the anxiety associated with key life events
Significant life events can make us anxious as well as stressed. Among other things, such as problems sleeping because our mind keeps churning, this can cause us to feel intimidated by the scale of something. For example, if we think about moving house, we see a massive mountain of stuff that must be sorted and packed, transported, unpacked and rearranged probably alongside a lot of DIY, decorating and carpet fitting.
Our brain reacts as though we’ve got to do it all, right now this minute and understandably we feel overwhelmed by the sheer scale and size of the task. Planning can help create a sense of how the task might be broken up to be dealt with in smaller chunks over time. And stepping back and using the mantra: "all I have to do now is…" can help us keep focussed on what it’s reasonable and possible to do in the here and now.
It also helps to identify familiar elements from the unfamiliar aspects of what you’re dealing with. There are lots of aspects of some things that you know how to do because you’ve done them before. For example, when my husband had his stroke I used to reassure myself by listing all the things that I already knew how to such as driving to and from the hospital, where to park when I got there, how to dial my friends phone numbers when I needed to talk.
Researching the less familiar aspects can help make them feel less strange. Even now, when I’m going to a place I’ve not been before I’ll research the routes I’ll need to use to get around using Google maps or something similar so I’ve got some idea of what the landmarks look like. If it’s possible to break the new aspects into smaller pieces that can be practised, that also helps to reduce the stress and anxiety that comes from dealing with the strange, rare and overwhelming.
The role of kindness and compassion
Rather than getting impatient for feeling a bit lost and confused, directing some compassion, tolerance and patience towards ourselves can be helpful. One of the kindest questions we can ask ourselves, one that really cuts to the heart of what we (or someone we care about) is finding difficult is:
"What troubles you the most about this situation?"

It can be surprising what sits at the bottom of a problem and where action really needs to be taken. You might think you already know the answer, but we all respond differently to major life events. It’s always a useful question to ask ourselves and/or others.
It can also help to think about the mindset with which we are approaching the life event. If our self-talk is very negative, that in itself will make things harder for us by ramping up the stress. That said, it is useful to acknowledge that something is difficult for you, but dwelling on that aspect is far from helpful. Research suggests that using your top three personal strengths when dealing with stressful situations and/or life events improves your confidence, leading to an increase in your feeling of mastery over at least some aspects of the situation.
If that feels too much, then borrowing from mindfulness can be helpful. I particularly like the aspect of friendly curiosity – the act of suspending your beliefs or mentally bracketing what you think you know about a situation in favour of exploring it with a view to getting to know and understand it properly. Anxiety often arises because we don’t properly understand something, taking the time to properly consider it can be helpful. If nothing else, it can help create time for you to appreciate what elements of it might be at least a little familiar and therefore for which you have some strategies to draw on.
Strategies to help you feel grounded in the face of significant stress
Last, and by no means least, if the whole thing feels strange, unfamiliar and overwhelming, then having some strategies to ground yourself can be helpful.
They can take many forms depending on what you’re trying to achieve. The simplest requires simply taking a big deep breath in and then letting it out very slowly. Sometimes, taking one breath is enough, other times you might need to do two or three. Breathing helps bring us back to ourselves and can settle and calm us.
Strong feelings of overwhelm can also be countered by creating a strong focus such as smelling (or sucking on) an extra strong mint. Likewise, pushing your feet hard into the floor or gripping the edge of something very hard. And while journal writing and artwork to help understand the swirling emotions can help for some people, for others soothing movement works better. Somatic movement, where you move slowly and gently from side to side or backwards and forwards in time to some slow and gentle sound can be very effective in returning you to yourself when you’re feeling stressed and overstretched.
No-one can escape major life events. There’s going to be something that happens at some point. It feels unfair that the Universe isn’t ordered in a way that says that if you’re already dealing with a significant health condition, you shouldn’t have to deal with anything else on top. But sadly, the world doesn’t work like that. What the world does have, is The Pituitary Foundation – a place you can go to talk to others who might have had similar problems to deal with. And a place where you can get advice about how to manage your pituitary condition in the face of stressful situations.
Prefer to watch instead of read? This blog post is also available as a video, which you can find below.
More about the author...

This blog post was written by Dr Sue Jackson, to go alongside her talk, titled 'Managing Life Changes.' Both this blog post and the talk were created for Pituitary Awareness Month 2025, as part of our 'A Lifetime of Hormone Health' campaign.
Dr Sue Jackson is an independent chartered psychologist, specialising in the link between mental and physical health. She is also a member of our Medical Committee, and provides essential support and insight to many areas of our work.

I’m 47 years old and it has been 17 years since my first symptoms and I guess I have at least another 17 years of brokering a truce with my pituitary gland. Hence my 'middling' status.
I have ‘controlled Cushing’s disease’. I’ve had two semi-successful pituitary surgeries and six weeks of radiotherapy, which completed on Halloween 2022. The last three years have been quiet - no signs of the feared regrowth or of the predicted pituitary failure. We watch and we wait.
Across the board it’s a mixed bag of changes. I am producing healthy amounts of cortisol myself (no steroids - yay!) and I am only replacing thyroxine and vasopressin BUT I still have most of my symptoms. I’m oppressively fat, I’m frustratingly weak and my blood pressure is worryingly high. Thankfully the oedema in my ankles is better as long as I keep my feet up regularly.
Some small wins - I no longer bruise so readily, the purple stretch marks on my tummy have turned silver and my head hair is gradually thickening and growing again. My chin hair lingers sadly… The radiotherapy caused my toenails to be crumbly until quite recently, so I can now wear sandals with pride!
How do I fill my days?
In a nutshell, I’m currently fully retired. Not quite how I imagined spending my 40’s but here I find myself!
I used to be a primary school teacher and, between surgery one and surgery two, I tried a gentle return to school. I took on roles as an intervention tutor, a supply teacher and then a part-time PPA (planning, preparation and assessment) teacher. In all those roles, I could get away with sitting down quite a bit and there were no break duties etc but quite frankly I was barely managing and it wasn’t sustainable. During the weeks after surgery two in March 2022, I came to the realisation that teaching as I knew it was over for me.
As it happened a close family member died during my treatment and just when I’d run out of earning power, a block of money arrived in my life. Quite frankly, I would rather have kept my teaching job and said family member but it was not to be. As a result, I have a mid-life pension. It won’t last forever and I’m not rolling in it but it’s enough to fund my rehabilitation efforts and protect me from having to rush the process.
In terms of my week, I spend about 70% of my time engaged in what I call ‘body management’. Therapeutic things like sessions in the swimming pool to get my joints moving, yoga and meditation to sooth my bruised brain, lymphatic massages for my oedema and talk therapy to help me make sense of everything that has happened.
The remainder is spent doing musical activities. Before I was a teacher I was a french horn player - orchestra tours, solo recitals, auditions etc etc. This revival of a past self has somewhat crept up on me. It started 2 years ago when my yoga teacher suggested we include meditation to music in our sessions. She would curate a playlist of her choosing and I would sit in my wheelchair, close my eyes and engage in deep listening. It felt like I was visiting a far-off place of sacred importance without having to move a muscle (phew!).
Looking ahead…
Since those sessions, my musical environment has expanded somewhat. I attend concerts as much as I can and I’ve joined a choir. I’m having one to one singing lessons, I’m about to start song-writing lessons, and last Christmas I visited my father abroad to both say hello and to extract my much-neglected french horn from his loft. I’m not quite ready to get it out of its case yet but suffice to say that I’ve got the number of a local brass instrument repairer and when the time is right my newly serviced Yamaha 867D and I will reunite.
As for what happens next, we have no idea if my body will ever gain the kind of metabolic agility that I once enjoyed. I remain realistically optimistic, patient and open to infinite possibilities.
I guess that’s all that one can do in ‘the middle bit’.
What is the difference between branded and generic medications?
Branded medicines are made by the company that first developed the drug. Once that company’s rights to the medicine (called a patent) run out, other companies can make their own version – this is called a generic medicine. Generic medicines must contain the same active ingredient as the branded version, in the same strength, and work the same way in the body in order to be approved for use.
Are generic medications equally effective as branded medications for people with pituitary conditions?
Yes, generic medications contain the same active ingredient as the branded version, which means they should work in the same way to treat your condition. However, the non-active ingredients – like colouring, flavouring or bulking agents – may be slightly different. These don’t affect how the medicine works, but in rare cases, some people might notice a difference if they’re sensitive to certain ingredients. For most people, generic and branded medications are equally safe and effective. If you have any concerns or feel different after switching, it’s always a good idea to speak with your GP or pharmacist.
Can I ask my GP for branded medication, or should I speak to the pharmacy?

If your prescription is written using the generic name, the pharmacist can choose which version (or brand) to supply. This usually depends on what they have in stock and what is cost-effective. You can ask the pharmacist if they have a specific brand, and they may be able to give it to you – especially if the price is similar. However, they don’t have to supply a certain brand unless it’s written on the prescription. The best way to make sure you always get the same brand is to speak to your GP. If your GP feels a particular brand works better for you, they can prescribe it by name.
It’s also worth noting that some medications are “brand-specific” – this means they should be prescribed and taken as a particular brand because small differences between versions might affect how well the medicine works or how your body responds. Your GP or endocrinologist will take this into account when prescribing.
I’ve been told I need extra hydrocortisone for ‘sick day rules’, but I’m struggling to get more on my prescription. What should I do?
Yes – it’s very important that you have enough hydrocortisone to follow the ‘sick day rules’, which usually means doubling your dose during illness, infections, or times of physical stress. To do this safely, you need to have extra hydrocortisone available at home. If your monthly prescription only gives you just enough for your regular dose, you should speak to your GP or practice team. Explain that you need a small reserve to manage illness safely and ask them to make a note on your medical records. If you’re still having difficulties, your endocrine team may also be able to support your request with a letter to your GP.
Should my repeat prescriptions from the GP be monthly or every 2 months?
This can vary depending on your individual needs and the practice’s prescribing policy. In many cases, it’s possible to receive a two-month supply of your medication, but this is up to your GP or prescriber’s discretion.
Can I have my prescriptions delivered from the pharmacy? I have trouble walking to collect them.
Many pharmacies do offer a delivery service, especially for people who have difficulty getting out to collect their medicines. However, this is usually a private service, so it’s up to each individual pharmacy whether they provide it and whether there is a charge.
How can I keep track of my medications and any changes to my prescription?
Managing medications for any condition can be challenging, especially if your doses change over time. Below is listed some helpful ways to stay organised:
- Keep a medication list: Ask for a printout from your surgery team or pharmacy and make sure to request an updated list whenever something changes. Bring the list to appointments to help your healthcare team
- Use a pill organiser: These can be really useful for keeping track of daily doses, especially if you’re taking multiple medications. However, if you ever need to go into hospital, it’s important to bring your medication in their original boxes with the pharmacy label showing the prescribed dose and instructions
- Set reminders: Phone alarms or medication reminder apps can help you stay on schedule
- Record changes: Keep a note of any medication changes, why they were made, and the date. You can use a small notebook or your phone’s notes app

Download our Sick Day Rules Table
You can download this table of the steroid Sick Day Rules, to take with you on the go
Download nowPrefer to watch rather than read? At the bottom of this page, you can access a recording of a talk on this topic delivered by Prof Pinkney.
Introduction
Conditions affecting the pituitary gland, and other endocrine glands, give rise to a notoriously wide range of symptoms. People ask endocrinologists all sorts of questions. Many concerns relate to impaired energy, stamina, and everyday quality-of-life. Over the years, one of the commonest concerns I have heard is about weight gain. I’m asked whether this has resulted from the underlying endocrine condition or perhaps the medicines that I have prescribed!
The majority of diseases affecting the pituitary gland have some impact on weight, such as Cushing’s disease and the hormone deficiency states of hypopituitarism. However, weight gain from pituitary disease is usually relatively modest. However, one group of conditions that stand out as causing more substantial weight gain are those that affect the hypothalamus. These can be primary diseases of the pituitary, or other disorders of the hypothalamus such as tumours. The hypothalamus is an area of the brain that plays an important role in the control of appetite and body weight, and when disturbed through disease processes, substantial weight gain is a relatively common result.
Unfortunately, in a world where two thirds of people are overweight, and over one quarter are obese anyway, it is not surprising that many people with pituitary conditions are overweight or obese, not primarily as a result of the pituitary condition, rather for all the many other common reasons that we gain weight. Some people are more predisposed from a young age, as a result of their genes, but also the behaviours and habits that have been learned from parents, or that arise in the home environment. Gradual weight gain often results when the diet is out of balance, often with excessive food portions, sometimes poor food choices, and frequently as a result of eating when not hungry, as in situations of stress, emotion or boredom. Having said this, most people find it very difficult to control body weight in a world where many of us are relatively inactive, and highly processed foods are major components in most people’s diets.
Weight control - what are the options?
Whenever I am asked for help with weight loss, it is important to understand the likely causes. I first consider the possible contribution to weight gain of the underlying endocrine disease, any associated abnormalities of hormone levels, and whether adjustment of endocrine treatment is necessary. Sometimes this is the case, although with weight gain in most endocrine disease being relatively modest, it is always necessary to consider the many other common factors that usually lead to weight gain in everyday life. At our centre we also run a large weight management service for people with more severe obesity, and it turns out that endocrine factors as causes of severe obesity are relatively rare. Whereas it is all of the other common factors related to day-to-day dietary behaviour and physical activity that are usually the more significant factors. These factors always have to be considered, even if there has been an endocrine contribution to weight gain.
A variety of different treatments can be used to bring about weight loss. For people who are overweight, or at lower levels of obesity, it is usually possible to achieve significant weight loss through relatively simple modifications of day-to-day lifestyle. Undoubtedly, this requires commitment, and to maintain long-term changes, but this is the traditional cornerstone of weight management, and without commitment to this principle treatments are often ineffective. Another approach, that can be combined with behavioural and lifestyle change, is drug treatment. For many years the available drug treatments for weight loss were not particularly effective, but now there is a new generation of drugs that are significantly more effective and offer the possibility of more substantial weight loss. Not surprisingly, there is now huge interest in these new treatments.
New drugs - new treatment options for weight loss?
The two new medicines available for weight loss are Wegovy (Semaglutide) and Mounjaro (Tirzepatide). Availability of Wegovy was limited throughout 2024 due to supply problems, and it was not widely available in the NHS. Mounjaro has been reviewed by NICE and it is expected soon to be available for use in the NHS. Perhaps the main question about these medicines is whether and how they can help people to achieve and maintain long-term weight loss, because the clinical trials have shown that most weight is usually re-gained within one year of stopping treatment. If this happens in clinical practice, this would be demoralising, probably not a good use of money, and repeated cycles of weight loss and regain may also be harmful for health. The NHS will be expected to follow NICE guidance on the use of these drugs, both in terms of who is eligible for treatment, and the need to stop treatment in people for whom it is proving ineffective and not achieving weight loss.
How can I try drug treatment for weight loss?
This would require advice from your GP or endocrinologist. Currently, access to treatment varies, and in many areas remains limited. At present the NHS use of Wegovy is restricted to those with more severe obesity (body mass index of greater than 35), accompanied by one or more weight-related common health problems. Although endocrine diseases often cause some degree of weight gain, the question will be therefore whether that weight gain has caused other health problems such as diabetes or high blood pressure. Accordingly, you would need to have a medical assessment of eligibility for treatment. Currently this drug is only to be prescribed from specialist weight management clinics and for a maximum period of 2 years. Mounjaro will also begin to become available in 2025, also for those with above BMI 35, with other weight related health problems. It seems likely that Mounjaro will prove somewhat more effective than Wegovy for weight loss, although that is not to say that Wegovy is necessarily an inferior choice for many people, depending on the amount of weight loss that is sought. Mounjaro can already be prescribed by GPs as a treatment for diabetes, and NICE will be recommending that GPs will also be able to prescribe this drug for weight loss, without any limit on duration.
Why is access to drug treatment currently limited?
A major challenge for the NHS is that the demand for these new drugs is so high that it is neither possible for the country to afford the cost of the drugs if they are to be given to everybody who is eligible, nor does the NHS have sufficient staff and capacity to see, assess and monitor the treatment of so many people. This is a global challenge, and not just one for the UK. Accordingly, in the NHS it is going to be recommended that treatments are made available with the gradual rollout over the next few years. It is envisaged that the first group of people to be eligible will be those with serious and urgent weight-related health problems, such as needing urgent treatment for life-threatening conditions, such as heart surgery or a kidney transplant. After this initial rollout, which is expected to take about three years, a larger group of people with BMI over 35 and significant weight-related health issues such as diabetes, high blood pressure, and the range of other conditions, will become eligible for treatment. What this means is that most people with endocrine diseases, whether or not these have contributed to weight gain, are not likely to be eligible for treatment in the near future. The main exceptions are likely to be for people who also have other serious weight-related health problems. Therefore, potential eligibility for treatment would be considered by GPs in the first instance. It is also worth appreciating that many GPs currently have little capacity to begin assessing and treating obesity, but it is hoped that this will change in the years ahead with more investment in these services. There is also some variation around the country in eligibility and availability of drug treatment. Most areas of the UK currently have relatively little availability, although it is hoped that this inequality will begin to improve.
Should I purchase drug treatment privately?
The drugs can be purchased privately, and there are a range of commercial weight management services that are able to assess obesity and where appropriate start treatment. Over the past two years this has been the main way that people have been able to access these drugs, and this remains one good option. Clearly the full costs of treatment have to be borne, and for many people this is not necessarily straightforward, although on the other hand many people make the choice to prioritise weight loss over some of their other expenditure. If treatment is purchased privately, as with NHS treatment, a key issue for consideration is what happens after treatment stops, and whether it will be possible to maintain dietary and lifestyle changes that will perpetuate the weight loss that has been achieved.
What side effects can be expected?
There is no reason to expect that patients with pituitary diseases will be any more at risk of side effects. Most common effects of this class of drug are gastrointestinal, such as nausea, vomiting, tummy pain, diarrhoea and constipation. These affect many people in the early stages of treatment, but usually subside. However. they can persist for some people and lead to stopping treatment. The main potentially serious side effect that has received a lot of discussion is pancreatitis, and while there is still some uncertainty about the cause of this, it is currently considered that this is usually caused by gallstones resulting from weight loss, rather than the drug itself. All in all, this family of drugs look to be relatively safe and well tolerated, and appears to represent a significant step forward in weight loss treatment.
Key points
- Whether or not you are eligible and suitable for drug treatment requires a medical assessment. This is especially the case for people with pituitary disease, who have more complex medical histories and treatment needs. An endocrinologist may confirm your eligibility and suitability but at present might not be able to prescribe the treatment for you. This may vary locally
- If you are thinking of accessing drug treatment privately, remember that the prescribing doctor will not have access to your medical records. People with pituitary diseases usually have complex medical histories, hormonal disturbances, and are often taking many different treatments. For this reason, it is best to discuss this first with your NHS doctors rather than going straight to a private provider
- Drug treatment is not necessarily the best option for all people. Some may be better off considering other treatments such as bariatric surgery. In order to assess the available options and to choose between them it is usually necessary to be referred to a specialist weight management clinic
- If drug treatment for weight loss is commenced, it should be used in conjunction with a programme of dietary change and increased physical activity, aiming to bring about and maintain long-term lifestyle changes. Drug treatment alone is not a quick fix. Without commitment, most people experience gradual weight regain after treatment is stopped. The long-term effects of treatment are not currently well understood, or whether long-term treatment is necessary in order to avoid weight regain
Professor Jonathon Pinkney recently delivered an online talk discussing weight management and options for treatment. The recording of this talk is available below.
Introductory idea: The 'dance of the everyday'
Psychology tells us that most of what we do each day is done by rote or habit, without us really having to think much about it. Something I call the ‘dance of the everyday’. Just as in a dance, we must learn the routine and how it fits with the pattern of the music and, if we have one, how our family behaves (their strengths and weaknesses), so in life.

A pituitary condition can disrupt the rhythms of life, imposing a new order that can be difficult to adjust to. The disruptions can be so significant that the person with the condition can end up feeling alienated and confused by the changes they’re experiencing, misunderstood and disbelieved by others, leading to the loneliness that is social isolation. How does someone end up there, and what can be done about it?
The difficulties of diagnosis
Some of the problems could be said to start from diagnosis. It can be stressful, shocking and traumatic to be told that you have a brain tumour. Pituitary tumours are mostly benign (i.e., non-cancerous), but you may not know that when your diagnosis is first communicated to you.
Say ‘tumour’ to most people and they will assume they have cancer. With the pituitary being in the brain, being told you have a pituitary condition can conjure up some very scary mental images for people. For all that doctors aim to be very careful in how they provide the diagnosis to patients, it’s inevitable that there are going to be some people who end up feeling shocked and, possibly, traumatised. Stress is highly communicable; as humans we’re wired to pay attention when other people are stressed, because if something is affecting them it might have implications for us too, so any shock and trauma is likely to ripple through family and friends.
When you’ve experienced something traumatic and stressful, it can really help to be able to talk to others who understand what’s happened to you. Judith L Herman in Trauma and Recovery talks about the importance of community in helping people to recover from traumatic experiences. On page 101, she observes that,
‘In ordinary bereavement, numerous social rituals contain and support the mourner … By contrast, no custom or common ritual recognizes the mourning that follows traumatic life events.’
On the following page she goes on to say:
‘Sharing the traumatic experience with others is a precondition for the restitution of a sense of a meaningful world. In this process, the survivor seeks assistance not only from those closest to her but also from the wider community. The response of the community has a powerful influence on the ultimate resolution of the trauma. Restoration of the breach between the traumatized person and the community depends, first, upon public acknowledgement of the traumatic event, and, second, upon some form of community action.’
Part of the problem with pituitary conditions is that they’re not easily understood by others. Unlike cancer, which most people will have some knowledge of these days, most people probably haven’t heard of the pituitary, and won’t know what it does, how important it is, or that there’s a set of diseases associated with it that can be far-reaching in their effects. Some healthcare professionals take the idea of patient-centred care to mean that they only ever talk to the patient, but someone who is shocked and stressed can’t take in information properly. So, a patient’s understanding about their condition and what’s going to happen to them next might be quite limited in the early days.
For conditions as complex as pituitary conditions, this is not good. Patients face a gamut of different tests and from early in the process, pituitary patients need to be working towards becoming experts in their condition. That’s a lot to take on, and being pointed to The Pituitary Foundation where you can find out more information about what’s happening to you would be very helpful, but unfortunately far from being directed towards The Foundation, lots of people are left to stumble over it themselves.
Chronic conditions and 'uncertainty'
As a species we’re very good with cyclic change – we’re used to the sun coming up and going down, getting ill and getting better again. Even with cancer these days, we’re used to the idea that things are curable albeit after some gruelling treatments and we expect those who survive to get back to pretty much how they were before. And that goes double for common illnesses such as colds and flu and the aftermath of accidents resulting in broken bones where the treatments are much less demanding on the patient. But, a pituitary condition is a long-term health condition that can’t be cured, it can only be treated. The idea that someone might be so affected by their condition that the outcome is uncertain and ‘getting better’ might mean that their condition is ameliorated by drugs but that they can’t get back to normal functioning can be somewhat mind-bending for both the patients and their family, friends and wider community.
Humans aren’t good with uncertainty. It’s much easier to support someone through something if you know how long it’s going to last for and what to expect along the way. Pituitary conditions can take people into unknown territory. The conditions and their treatments can change how someone looks, as well as how they react and respond to things. Some people will end up with crushing fatigue that limits what they can physically do and brain fog that affects what they can think about. Pituitary patients can be shocked and surprised anew when confronted by reactions that they don’t recognise in themselves. They can start to wonder if they’re going mad on top of everything else they’re dealing with. Their family and friends can find it very confusing and difficult to understand too.
Adjusting to uncertain situations
We’re used to the idea that being ill is a consistent state, the idea that someone might have a condition that fluctuates such that what they can do in the morning is different to what they can manage to do later in the day, and that that can shift and change from day to day is bewildering and confusing for all concerned. When someone is ill with flu it can be easier to shift from the ‘dance of the everyday’ where everyone in the household does their usual thing, to the family dancing attendance on the person who isn’t well.
But the timescales involved in pituitary conditions can leave family members wondering how long they might have to dance attendance for. The uncertainty around what support is needed and for how long might not be known by the patient or their family and that can put tremendous pressure on how the family functions. It’s very hard to be disconnected from yourself and your family, thrown out of all your everyday routines and habits and methods of engagement and profoundly unsure about how long that situation will last. Death is straightforward – the person isn’t there anymore – but someone who is profoundly changed but still present; that’s quite a conundrum for all concerned.
'Someone who is profoundly changed but still present; that's quite a conundrum for all concerned.'
How does 'community' play a role in this?
The Pituitary Foundation offers a community that genuinely understands what it’s like to live with a pituitary condition. They have a lot of useful information as well as other people to talk to. Some of those people are healthcare professionals whom you can ask for advice about how to understand what’s happening to you and what might be next on your treatment journey. But there are other people who’ve been on this journey before you who will also have insights to share.
here’s a tremendous psychological relief that comes with knowing that it’s not just you that finds it difficult to understand and to live with. And that support and information is there for family and friends too. In dance terms, it reminds me of learning a complex country dance where the people who already know the dance explain it to you in ways you can understand, then hold your hand as you gradually learn what’s required of you.

Maintaining good wellbeing with a long-term health condition can be challenging. Having a pituitary condition can impact all areas of your life and make it difficult to stay healthy whilst navigating complex things like relationships, conflict and communication.
In this blog post, Dr Sue Jackson (Chartered Psychologist) explores the role of assertiveness in healthy communication and wellbeing, and the ways people with chronic health conditions can sometimes struggle with this. A video of Dr Jackson's talk on this topic is also available at the bottom of this page.
The art of assertiveness
Lots of people confuse confidence with self-esteem, or assertiveness (I know I did when I was younger). While it is closely related to both of those things, it isn’t the same thing.
Confidence is the extent to which we trust ourselves, particularly our abilities, personal qualities and judgements. It’s about both what we do and how we feel about what we do, particularly the extent to which we are comfortable with the various skills we have. Assertiveness is a social skill that relies heavily on effective communication. To be assertive means learning to honestly express our opinions, feelings, attitudes, and rights, without feeling anxiety and fear, while at the same time acknowledging other people’s rights, thoughts and wishes.
Assertiveness is a communication skill (so it’s related to confidence), but it’s based on how well we understand our needs and boundaries (hence its relation to self-esteem). It’s the art of treating others with the same love and respect that you would like to have extended to yourself. It’s not about forcing your views on other people or being aggressive towards others. It is about taking responsibility for the choices that you make and the consequences that follow from those choices when communicating with others. Assertiveness works best when you’re clear about what outcome you would like to achieve from the conversation/situation you find yourself in.
Assertiveness issues for people with pituitary conditions
I think people with pituitary conditions can struggle being assertive for several reasons. There are a lot of pituitary conditions and they can be complicated to manage and live with. Quite often family, friends and colleagues may not have heard of either the pituitary gland or the various conditions that can be associated with it before and therefore not understand what it means when you try to explain your condition and its management to them. Pituitary patients often say that healthcare professionals don’t provide them with good information to pass onto others, which doesn’t help. Trying to explain something complicated when the condition you have causes fatigue, brain fog, problems with memory and concentration is a tall order. It can be stressful and difficult to ask for help and understanding especially with fluctuating symptoms. You can get pushback – "You managed alright yesterday" – because as a society we’re encouraged to have a work ethic that means you don’t stop for a little thing like being unwell. Other people can think that they know better than you, or they don’t want to believe you because if they did then they’d have to do something about it and right now they may not be able to.

Being assertive
The Bill of Assertive Rights was first suggested by Manuel J Smith in his 1985 book When I say no, I feel guilty. The bill comprises a useful list of the different ways in which we’re all allowed to be assertive. Some of them (for example, the right to privacy) are easier than some others (for example, the right to be heard), which depends on gaining the cooperation of others. There are some (such as the right to be treated with respect as a capable and equal human being) that can easily be infringed by others when we’re not well, making it hard for us to retain our voice, independence and agency. I think some of those problems stem from the fact that, as a society, we don’t have a good understanding of what it means to live with a chronic health condition.
We’re used to people having colds where we expect them to comply with what’s been dubbed ‘the sick role’. The key characteristics of the sick role – having symptoms that others recognise, being exempted from daily activities, seeking professional help where indicated, and wanting to get better – are totally appropriate for short-term bouts of illness. However, with chronic conditions there is no ‘getting better’; we’re in the realms of treatment and not cure and while some exemptions from activities of daily living can be appropriate for some people with pituitary conditions some of the time, it’s not going to be appropriate for all pituitary patients most of the time.
"With chronic conditions there is no 'getting better'; we're in the realms of treatment and not sure, and while some exemptions from daily living can be appropriate for some people with pituitary conditions some of the time, it's not going to be appropriate for all pituitary patients, most of the time."
Practice makes perfect
Assertiveness is a communication skill that takes practice to get right because it doesn’t always go according to plan the first few times you try it. I’ve seen it taught very poorly on some assertiveness training courses where people are basically being told how to be verbally aggressive towards others. One of the key aspects of assertiveness that often gets overlooked on such courses is that it’s about maintaining functional relationships. For example, you need to take responsibility for how you are feeling and be able to accept and hear that someone else may be feeling differently to you. You need to accept that even having heard you, the other person may not be able to respond to your communication or meet your needs right now.
Communicating effectively with others can be complicated and tiring. You may need to check that the other person understands what you are saying, which means you might need them to repeat back to you what it is they think you are trying to communicate. You can then clarify any bits they seem to be misunderstanding. Remember – we each use words in different ways and we tend to only half-listen to other people. Most of us during conversations are thinking about what we’re going to say in reply to what we’ve just heard rather than properly paying attention to what we’re being told. It can be tempting to up the ante by using exaggerated or colourful language, but that merely serves to stress both you and the individual that you are trying to talk to. We often spend time describing the things that are upsetting us, which is understandable if we want someone to understand where we are coming from, but if we only dwell on what we don’t want it can lead to confusion. The other person might struggle to see how they can help you, so using positive statements identifying what it is that you would like to see as an outcome can be useful. But doing that means you need to have prepared yourself beforehand to understand what a range of good outcomes might look like for you.
Assertiveness and boundaries in a relationship
If assertiveness is about communicating effectively within a relationship then how we see each other as humans plays a part in that communication. If we take a two-person example where two people both see themselves as being OK, then the communication is also likely to be OK. But where one person sees themselves as being OK and the other person as being much less than OK, problems can arise. The person who sees themselves as being OK can become quite critical, while the person who feels that they’re not OK can find themselves becoming defensive and blocked from communicating honestly with the other person. In situations like this, having some boundaries can be helpful.
There is always going to be some people in our lives who, for whatever reason, are struggling to see us as we’d like them to. It might not just be about health or illness issues, it can also be because others see us as performing a particular role in their life (for example, you’re always the helper) and they struggle to see us in any other way (right now, you’re the one that needs help). Having some boundaries in some areas of our life can be very helpful. There is a myth that having boundaries makes you mean and selfish but that’s not the case at all. Creating and understanding where our boundaries are is an important part of self-care. It’s easy to get sucked into spending time and energy doing things for entitled others but when you have a chronic health condition, it’s important to avoid over-giving and over-functioning. Doing more than is required will make you unwell and creates confusion for you and others about what your sensible and safe limits are.
Other ways of being assertive
There are some other things that also help with being assertive. For example, having or fostering an identity as a survivor rather than a victim and believing that there are things that we can do to help us to manage our feelings and to cope. It may not be easy or obvious what those things are though, which means lots of mistakes can be made which we will need to learn to forgive ourselves and others for. It can be a long process full of problems and that can make people feel downhearted. This is where the attitude of gratitude comes in – the ability to be able to recognise and appreciate what I call ‘the little gleams of sunshine’ that still exist and that you can still enjoy. Something as simple as watching a cat wash his ears, or seeing the sunlight sparkling through raindrops, or enjoying the feel of the support of your favourite cushion on the sofa.
Sources of support
Being willing to seek help with something as challenging to live with as a pituitary condition is a sign of strength, not weakness. It’s common to need support to work on your assertiveness, if for no other reason than to get some ideas about things you can try to help explain your condition to others. Although you might also want to discuss how to deal with tricky people in your life and whether and how to set some boundaries to help you with your self-care. So it might help to remember that The Pituitary Foundation has both telephone buddies and a helpline you can call, and they now have a new counselling service run by Rareminds.
Watch this talk below
Life with a pituitary condition can undermine your relationship with yourself, leading to low self-esteem, but what does that mean? What is self-esteem?
In this blog post, Dr Sue Jackson (Chartered Psychologist) explores self-esteem and the ways it can be impacted by a chronic health condition.
What is self-esteem?
According to Rosenberg (the author of one of the most used questionnaires designed to measure self-esteem), it is the word we use to describe and/or summarise our attitude towards ourselves. That attitude can be either positive or negative. I would add that it goes to the heart of what it means to be a person – the central beliefs we have about ourselves and the kind of person we each think we are or feel ourselves to be.
Definitions and descriptions of self-esteem

Before they started researching it, psychologists used to think that most people had good self-esteem. It came as something of a surprise to find that people with good, stable self-esteem (i.e., those who see themselves as good and worthwhile individuals pretty much all the time) are quite rare. For ease of reference, and because there are some misconceptions about what good self-esteem looks like, here’s a description. People with good, stable self-esteem are generally very comfortable with themselves, which makes them easy to be around, not least because you know where you stand with them. They love and accept themselves as they are, strengths and weaknesses included, although this doesn’t mean that they have an inflated opinion of themselves. They’re aware that they are human, that they make mistakes and get things wrong. They can accept constructive criticism without seeing it as a personal insult. Instead, they see it as information they can use to improve. They don’t feel the need to prove anything, which leaves them open to letting themselves have experiences from which they can learn without worrying what other people might think – they are simply willing to try things. They respect themselves, whilst also respecting others.
Over time it has become clear there are three different kinds of self-esteem:
- Good, stable self-esteem
- Chronically low self-esteem
- Variable or fluctuating self-esteem
Most people seem to have a good understanding of what poor self-esteem can be like and, when questioned about it, generally describe someone with negative and critical thoughts about themselves, troubled by uncertainty and self-doubt. That said, lots of people confuse self-esteem with confidence and assertiveness (I know I did when I was younger) and while it is closely related to both of those things, it isn’t the same thing.
Assertiveness is a social skill that relies heavily on effective communication. To be assertive means learning to honestly express your opinions, feelings, attitudes and rights, without feeling anxiety and fear, while at the same time acknowledging other people’s rights, thoughts and wishes. With a definition like that, it is easy to see why people think assertiveness and self-esteem are closely linked.
Meanwhile, confidence is the extent to which you are comfortable with the various skills you have. For example, there are some things that you are so confident at doing that you don’t even think about them as being skills anymore unless you must relearn them for some reason (for example, walking or making a drink). There are other skills where you are not so sure of your abilities and so you tend to think about them more, especially as regards your performance of them. For example, I’d say that I’m an OK cook but I’m aware that there’s a lot that I still don’t know how to do. Quite often people confuse what they can or can’t do with who they are and how they feel about themselves, which leads to fluctuating self-esteem. As an example, when they’re doing well they feel fine with themselves but if they make a mistake in performing a task, particularly if someone else points that out to them publicly, it can really dent their confidence. This can then lead to them having very self-critical thoughts and feeling bad about themselves.
Manifestations of low self-esteem
While most people find it very easy to describe low self-esteem, they may not be aware that it can manifest itself in several ways. There are those with low self-esteem who may wonder what use they are and who can end up feeling that the world would be better off without them in it. They can lack a sense of having any value as a person at all, feeling that others do not like them, love them or care about them. Despite this, they may be acutely sensitive to the needs of others and may put these needs above their own. Some people may go so far as to believe that the only time their presence is acceptable to other people is when they’re doing things for others – the idea of turning up empty-handed to someone else’s house for a cup of tea and a chat leaves them in a cold sweat. They may worry that they are unable to do things right or feel anxious if they are prevented from doing things for others, for example, because of ill-health.
Some people with low self-esteem dislike themselves so much it leads them to lash out and hurt others. Someone who is routinely very critical of others, who rarely has a good word to say about anyone, who always points out the errors you make but who is seemingly unable to give you any praise is quite possibly acting out of low self-esteem. Bullies quite often have low self-esteem and/or are very scared of other people. Their behaviour is an attempt to try and control others by cutting them down to size and keeping them off-balance.
Pituitary conditions and self-esteem
I think people with pituitary conditions can develop self-esteem problems partly because the various conditions, and their respective treatments, can change so much about what it means for them to be who they are. In short, some of the conditions cause changes to appearance and lots of the conditions cause problems with mood swings and emotional reactions. Many people may also struggle with fatigue and low energy, presenting them with difficult choices about what they can do, especially if the fatigue comes with brain fog and memory problems. All of this can leave someone feeling lost, unsure, worthless, hopeless and miserable.
Living with someone with a pituitary condition can trigger self-esteem issues for their support network too. Family members and friends can be surprised by their own reactions to living with someone with a long-term condition. It can be confusing, frustrating, and difficult – people report being surprised at how uncertain, worried, angry, and sad they feel. If this leads to arguments and unkind things being said and done, the shame and guilt can lead you to wonder just what kind of a person you really are.
Improving self-esteem
I would argue that the key to improving self-esteem is practising self-respect. There are many ways to do this so I usually suggest you pick one that looks the easiest to try and work on. For example, you could learn to listen to yourself – your opinions and emotions matter. They’re an important source of information about yourself and the world around you. People with low self-esteem often don’t treat themselves very well and the language they use towards themselves when they make mistakes is often foul and hurtful. Learning to treat yourself with patience and understanding could be an important first step for some people. Being polite towards ourselves is important for all of us, as research shows that the bad language and nasty names we employ towards ourselves cause stress and anxiety.
Some people might find it easier to start with attending to their physical needs as part of improving their self-esteem. This could look like taking a break when you're feeling tired, having a drink when you're feeling thirsty or looking after your nutritional needs appropriately.
If your self-esteem is very poor, it can feel terrifying to start to treat yourself with dignity and respect. You may have a very real fear that if certain people find out that you’re seeking to improve yourself they will slap you down. That fear can be so powerful that it can lead you to feel that it’s both easier and safer to stay as you are. To those people I would say two things. Firstly, it’s important to work on having some boundaries in your mind, such that you understand what is genuinely about you and what is someone else’s issue. And secondly, your relationship with yourself is allowed to be private. You’re allowed to talk to yourself kindly, to be loving and gentle towards yourself without telling anyone else that that’s what you’re doing. I often refer to improving self-esteem as something of a Secret Squirrel task, because it can be difficult for people to acknowledge or discuss with others.
Your relationship with yourself is allowed to be private. You're allowed to talk to yourself kindly; to be loving and gentle towards yourself without telling anyone else that that's what you are doing.
Sources of support
The relationship you have with yourself is arguably the only one that you will have that will last your whole life. If it’s a troubled relationship, it’s worth doing some work on it to try and improve it even though for lots of us that’s much easier said than done. To try and help, The Pituitary Foundation has a booklet called Relationships & Communication that starts out considering the relationship you have with yourself and how to improve, it if it isn’t good, before moving on to addressing relationships with other people.
It’s not unusual to need support to work on your self-esteem (I know I did when I was younger), so remember that The Pituitary Foundation has both telephone buddies and a helpline you can call, and they now have a new counselling service run by Rareminds.













