My story starts in 2020. I had headaches, dizziness, was constantly tired and generally rubbish. I had an MRI and they found a tumour; I had a pituitary macroadenoma. The very thought of a tumour was alarming and it was in Covid times, therefore I wasn't able to see anyone for support. A month previous, I found out I was pregnant and as you can imagine, I was filled with dread and so many questions.

I was told by my employer that due to my illness they could not carry on my employment- another whack in the face! My whole life as I knew it was uncertain. I was scared and felt alone. I also suffer from depression and anxiety and this was through the roof. I tried to maintain a positive mentality for my twelve year old daughter; it was hard.
I was told that I needed surgery however, due to the pregnancy, this could not happen until after I gave birth. I was also told that it was a rarity to get pregnant whilst having this diagnosis. As such, a case study has been written. I had regular scans and, towards the end of the pregnancy, the tumour was getting larger. Apparently this can happen due to the pregnancy hormones. The symptoms were getting worse and my sight was deteriorating. The surgeon said they could not wait any longer and I was booked in to have a caesarian section five weeks early. I was informed that I would be unable to breast feed as this would also increase the tumour. I felt a failure. I wanted to give birth to my son naturally and feed him. My mental health was crashing.
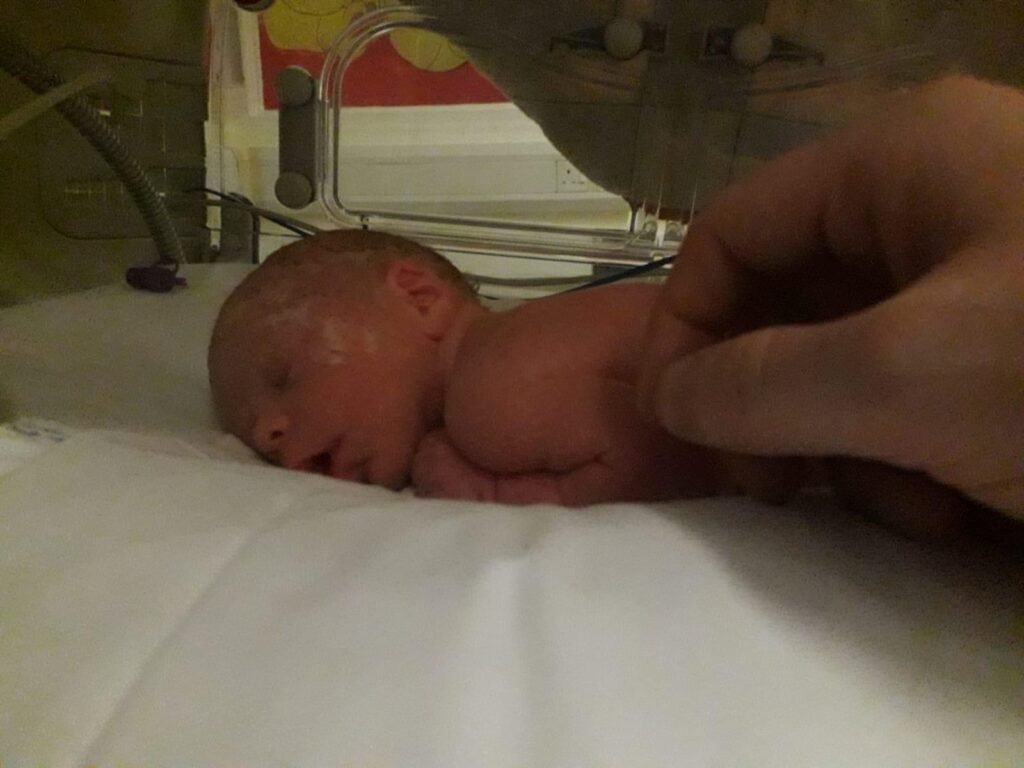
I was informed that I would be unable to feed him as this would also increase the tumour. I felt a failure. I wanted to give birth to my son naturally and feed him.
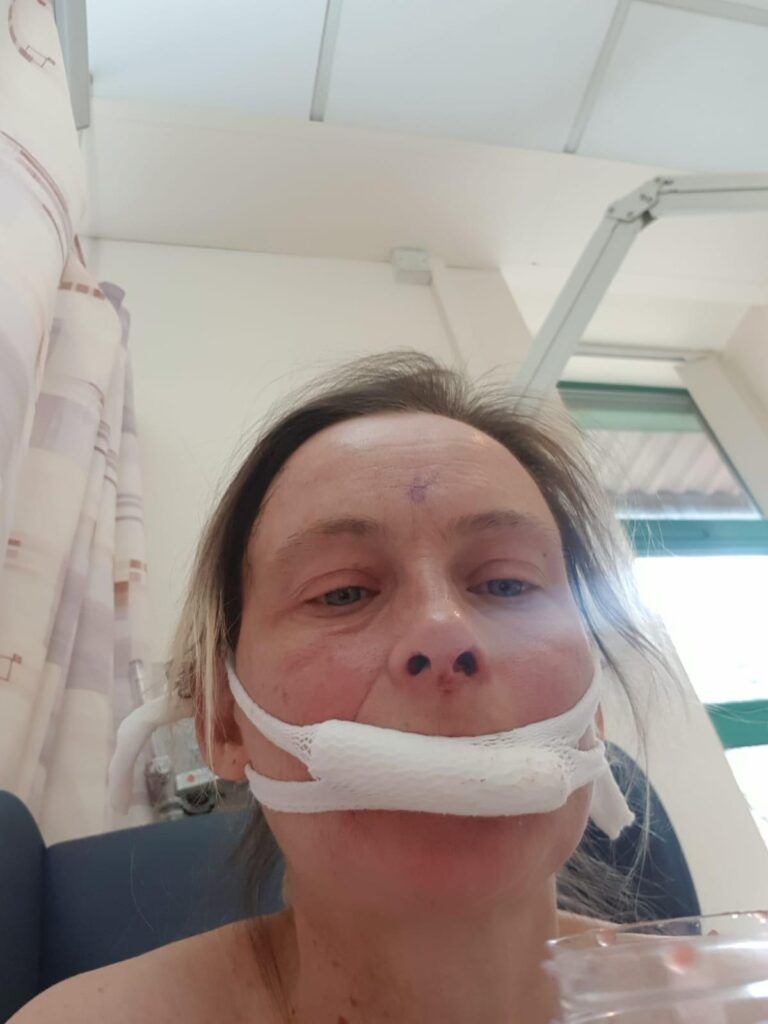
Within two weeks of giving birth to my son, I was in a special neurological hospital having the tumour resected. I could not have asked for better treatment and reassurance. Due to Covid, I was unable to see my partner or children. I came out of hospital six days later and it was a long recovery because of the caesarean, brain surgery and depression.
I have not worked since. I am still constantly tired. If I have a productive day, the next day I am wiped out. This would make it hard going into a job as I couldn't be reliable. This upsets me, as I am skilled and proficient as a financial trader and market manager.



Life is not the same. I have no sense of smell or taste, however if I ask myself how grateful am I? The answer is easy. I look at my children, I breathe in the cold air, watch the birds flying, I am beyond thankful I am here.

I’m 47 years old and it has been 17 years since my first symptoms and I guess I have at least another 17 years of brokering a truce with my pituitary gland. Hence my 'middling' status.
I have ‘controlled Cushing’s disease’. I’ve had two semi-successful pituitary surgeries and six weeks of radiotherapy, which completed on Halloween 2022. The last three years have been quiet - no signs of the feared regrowth or of the predicted pituitary failure. We watch and we wait.
Across the board it’s a mixed bag of changes. I am producing healthy amounts of cortisol myself (no steroids - yay!) and I am only replacing thyroxine and vasopressin BUT I still have most of my symptoms. I’m oppressively fat, I’m frustratingly weak and my blood pressure is worryingly high. Thankfully the oedema in my ankles is better as long as I keep my feet up regularly.
Some small wins - I no longer bruise so readily, the purple stretch marks on my tummy have turned silver and my head hair is gradually thickening and growing again. My chin hair lingers sadly… The radiotherapy caused my toenails to be crumbly until quite recently, so I can now wear sandals with pride!
How do I fill my days?
In a nutshell, I’m currently fully retired. Not quite how I imagined spending my 40’s but here I find myself!
I used to be a primary school teacher and, between surgery one and surgery two, I tried a gentle return to school. I took on roles as an intervention tutor, a supply teacher and then a part-time PPA (planning, preparation and assessment) teacher. In all those roles, I could get away with sitting down quite a bit and there were no break duties etc but quite frankly I was barely managing and it wasn’t sustainable. During the weeks after surgery two in March 2022, I came to the realisation that teaching as I knew it was over for me.
As it happened a close family member died during my treatment and just when I’d run out of earning power, a block of money arrived in my life. Quite frankly, I would rather have kept my teaching job and said family member but it was not to be. As a result, I have a mid-life pension. It won’t last forever and I’m not rolling in it but it’s enough to fund my rehabilitation efforts and protect me from having to rush the process.
In terms of my week, I spend about 70% of my time engaged in what I call ‘body management’. Therapeutic things like sessions in the swimming pool to get my joints moving, yoga and meditation to sooth my bruised brain, lymphatic massages for my oedema and talk therapy to help me make sense of everything that has happened.
The remainder is spent doing musical activities. Before I was a teacher I was a french horn player - orchestra tours, solo recitals, auditions etc etc. This revival of a past self has somewhat crept up on me. It started 2 years ago when my yoga teacher suggested we include meditation to music in our sessions. She would curate a playlist of her choosing and I would sit in my wheelchair, close my eyes and engage in deep listening. It felt like I was visiting a far-off place of sacred importance without having to move a muscle (phew!).
Looking ahead…
Since those sessions, my musical environment has expanded somewhat. I attend concerts as much as I can and I’ve joined a choir. I’m having one to one singing lessons, I’m about to start song-writing lessons, and last Christmas I visited my father abroad to both say hello and to extract my much-neglected french horn from his loft. I’m not quite ready to get it out of its case yet but suffice to say that I’ve got the number of a local brass instrument repairer and when the time is right my newly serviced Yamaha 867D and I will reunite.
As for what happens next, we have no idea if my body will ever gain the kind of metabolic agility that I once enjoyed. I remain realistically optimistic, patient and open to infinite possibilities.
I guess that’s all that one can do in ‘the middle bit’.
This article was written by Sammy Harbut, an occupational therapist who provides vocational support and advice to individuals with long term health conditions.
Research shows work to be beneficial for both physical and mental health and wellbeing. Having routine and purpose can be very positive and finding a sense of 'normal' is often helpful for people after a diagnosis of a long-term health condition. However, returning to work after a long period of absence may feel scary. You may have questions about what will be expected of you, or what support is available to help you adjust and find your feet.
Returning to work often involves a mixed approach that draws on support from your healthcare team and your employer. You can read more about this below.
Role of the employer

Employers obviously play a very important role in helping you return to work, through making your work environment and routine more accessible and supportive. In doing so, employers need to consider reasonable adjustments that can be made to support employees with long-term conditions.
Following any diagnosis and treatment, it is important to plan a structured return to work. A phased return-to-work plan should include input from both employer and employee, with support from an occupational health department, if available. Employers are required to consider reasonable adjustments and a phased return to work under the under the Equality Act 2010. You can read more about reasonable adjustments here.
What do you need to be aware of when having a return to work conversation?
It is entirely your choice whether or not you talk to work about your health problems and support needs. You do not need to disclose anything you do not want to. However, if you would like your employer to make reasonable adjustments to support your return to work, it's important that they understand what support and changes you may need.
A successful conversation about this might include:
- Any concerns you have about returning to work and the impact this could have on your condition
- Possible changes to your confidence after your diagnosis and treatment
- Agreeing what you are, and aren't, comfortable sharing with other people at work
- Providing your employer with some information about your condition and treatment (if you wish to)
Following health issues, an employee is often the best person to know what further support they may require and
have good ideas on how to achieve this. Be active in your own return to work plan, think about the demands of the job and the support you will need as you return. You may not need to be 100% fit before returning to work, but can still work effectively with support. Reasonable adjustments should be negotiated with the employer, but remember any fitness for work guidance is ‘advisory’ and can be amended by the employee and employer. You may find you return to fitness sooner than expected or you may suffer additional health issues and consequently take longer get back to work.
The Allied Health Professionals (AHP) Health and Work Report
The AHP Health and Work Report is a form that can be filled out to detail what support an employee needs to be able to continue working, or return to work after absence. It is used by employees, employers and healthcare teams to collect this information, and share with employers. The report provides a consistent and nationally-recognised tool to advise employees on their fitness for work. It has been designed to provide information on the functional impact of a patient’s reported problem and to suggest options that may support the patient to remain in, or return to, work.
The AHP Health and Work Report includes details about what you as the patient can do, as well as highlighting
difficulties and suggest adjustments within the workplace to facilitate a return to employment. The advantage of an allied healthcare professional providing this report is they often have greater and more up-to-date knowledge of you than a GP, if they have been working with you. It is important to remember that any report is advisory. Either the employer or employee may choose not to take this advice or provide alternative solutions.
However, if a recommendation provides practical solutions which can be accommodated, this will improve the likelihood of advice being taken and better relations between employer and employee.
Recommendations in AHP reports should aim to be:
- Practical and easily understood without having a negative impact on other staff members
- Specific, easily achievable, realistic and timely, and with timescales for adjustments clearly stated
- Sensitive to any costs involved
- Personal to the individual. Simple but cleverly thought out recommendations can be very effective when personal circumstances are considered
Phased to return following treatment
It is a good idea to have an extended phased return to normal working hours, to give you time to adjust slowly. Anything up to eight weeks is appropriate. The phased return should be negotiated between you, as an employee, and your immediate line manager. This is because you will both have an awareness of the working environment and tasks that need to be completed. You should aim to start with a few hours a day, either in the morning or afternoon, and gradually build up this time over the weeks. It is not advisable to work overtime or take on extra duties during this period.
During the discussion period, it is also useful to carry out a risk assessment for returning to work. The risk assessment should not be too ominous - it is just a sensible set of procedures to ensure you are as safe as you can be. If you have a condition that requires emergency medication, such as emergency hydrocortisone injections, it can be helpful to talk about situations where this may be required and what your work needs to do/know to support you.
Things to think about in a risk assessment:
1.Location
Do you have a long way to travel before even getting to work? Any long distance which will use energy? Do you have access to facilities should you need them? Is there a quiet place you can go to within the workplace should you need to?
2. Medication
Do you need people at work to know how to adminster emergency medication? Will you be able to take your medication when needed and have access to whatever you need to do this? You might want to set an alarm on your phone initially too, as a means of ensuring you take your meds at the right time, as it is easy to forget if you are very busy.
3. Activities
This is perhaps the most significant, as your working day will need to incorporate breaks and downtime to allow you to build in regular rest periods. You should try to have a balance of different types of activity throughout the day.
We use different amounts of energy for different tasks. Mental tasks can be as exhausting as physical ones, so try to strike a good balance and don’t forget social activities, which also use energy, though are usually more enjoyable. Always try to pace all your activities - both during work time and in preparation of these. You can read our Fatigue Management Booklet for more information about this.
4. Equipment
Make things as easy as possible for yourself by ensuring all equipment you use is in good working order. If you can avoid lifting heavy items for long periods, then this will help preserve energy levels. If you are able to get others to help you, rather than you moving about a lot initially, this will help too.
5. People
Make sure you have a good support network around you. If you encounter a difficult situation, be aware that this will cause stress which is normally catered for by an increase in cortisol. If you are now reliant on steroids because you are adrenal insufficient, your body will be unable to respond to this extra stress.
Make sure that your line manager is fully aware that you will need some time and space to get used to your new routine whilst you are adjusting to working life again. As long as your return to work is gradual and planned, there is no reason why it should not be successful. You will need to get into a routine, but this will come with time (and patience) and managing your pituitary condition will become automatic.
References
- Bajorek, Z. Hind, A. and Bevan, S. 2016. The impact of long-term conditions on employment and the wider UK economy. The Work Foundation. Available here (Accessed 4th September 2025)
- National Institute for Health and Care Excellence, 2016. Workplace Health: Management Practices. Available here (Accessed 4th September 2025)
- Royal College of Occupational Therapists (2021) Specialist Work Section
- Royal College of Occupational Therapists (2021). The AHP Health and Work Report. Available here (Accessed 4th September 2025)








