Learn more about how to communicate well with your family and friends when it comes to ongoing and difficult health problems, in this article written by Dr Sue Jackson. A corresponding video of her talk on this topic can be found below.
Communicating With Your Loved Ones
Written by Dr Sue Jackson
Lots of us take our ability to communicate for granted. It might only be when you start having problems in getting your message across to someone else that you start to think there might be more to it than simply putting words in the right order. Communication difficulties, such as being misunderstood or disbelieved, are not uncommon for people with chronic health conditions. This article thinks about why that might be and looks at some things that might help.
The basics of communication
Communication is a skill that enables us to be able to relate to other people effectively. We need to be able to communicate to share ideas, explain to others what we need or want, to work out differences and areas of conflict, and to express our feelings. Since it’s a skill, it relates to self-confidence (in this case how comfortable we feel in talking about ourselves to other people) and because we’re talking about what we want and/or need (or feelings and such), communication also relies on assertiveness. Confidence can be thought of as the extent to which we trust ourselves, particularly our abilities, personal qualities and judgements. It’s about both what we do and how we feel about what we do, particularly the extent to which we are comfortable with the various skills we each have. Assertiveness is a social skill that relies heavily on effective communication. To be assertive means learning to honestly express our opinions, feelings, attitudes, and rights, without feeling anxiety and fear, while at the same time acknowledging other people’s rights, thoughts and wishes. A tricky line to walk and the subject of another article.
Communication isn’t just about what we say, which might come as something of a relief to those of us who aren’t so good with words. In fact, at just 7%, research suggests that the words we say make up the smallest part of our communications with each other. By far the largest part of our communication (60%, or getting on for two-thirds) is made up of our body language. The remaining third is the tone of voice we’re employing, whether that’s kind and gentle, sarcastic and cutting, or angry and domineering.
In most normal conversations, we take turns (although there are a few people who don’t seem to understand that a conversation should involve more than one person’s voice!). However, often we don’t really listen to what the other person is saying. What most of us do is to mentally start preparing for what we’re going to say when they stop talking, or (if we get a bit over-eager) we’ll jump on the end of their sentence before they’ve stopped speaking.
Acute versus chronic health conditions
You might think that communication about illness is just another ordinary kind of conversation and, if someone has a cold or some other acute problem like a broken leg, that’s probably true. We all have enough experience of common illnesses for there not to be much to discuss because we know what’s going to happen, both to the person with the illness and those of us who will be supporting and looking after them.
A chronic health condition is very different and could be described, in relation to pituitary conditions, as a series of events that kickstarts a process more akin to a marathon than a sprint that can last for months, if not years, or indeed for the rest of your life. Unlike acute conditions, where we’ve got used to quick diagnoses and effective cures followed by a return to normal functioning for the affected person, chronic conditions involve treatments rather than cures, and those treatments may not return the person to who and how they were before they were diagnosed. Added to which, the process of diagnosis may well have taken years.
A chronic condition can require close monitoring and regular adjustments to a medical regimen. This may involve regular check-ups involving blood tests and scans and patients may experience quite a lot of worries and concerns about what those results might say about how their condition is progressing. While people often describe it as battling or fighting, there are times when a chronic health condition is something to be managed and worked with rather than something to be fought with. While the process of diagnosis and treatment might be straightforward for some, for others their condition can keep recurring and instead of being straightforward, it feels like they’re trapped inside a revolving door of symptoms, diagnostics and treatments.
Communicating your condition to others
Understanding how to live with a chronic health condition isn’t necessarily straightforward whether you’re the patient or not. There’s potentially a lot to find out about and deal with. What you need to communicate to others may well be different as you move through the different stages of your condition. Take your time to prepare what you’re wanting to achieve from talking to others. Dwelling on what you don’t want can lead to confusion, so you might want to think about what would be helpful instead. You might also need to think about the following three things, too:
- Are you asking to be cared about and understood? (For example, you’re looking for expressions of love and support but you’re not looking for any ‘fixes’)
- Are you asking to be cared for and helped? If so, what is that would make a difference?
- Are you asking for both of the above?
If possible, choose a time so that everyone is in the best frame of mind for hearing what you have to say. I’m a lark (which means my energy is at its best first thing in the morning), while my husband is an owl (which means his energy is at its best later in the day). Conversations where we both need to concentrate are best done in the afternoon when our energy levels are more equal, which lends itself to fewer misunderstandings and, as a consequence, less arguing. We also help make things less confrontational by sitting side-by-side or going for a walk. Movement can be soothing and walking sets a gentle pace for a conversation.
You may need to check that the other person understands what you are saying, for example, you can ask them to repeat back to you what it is they think you are trying to communicate. You can then clarify any bits they seem to be misunderstanding. Remember – we each use words in different ways. A good example is when a doctor says you’ll be better after the operation, but what they might mean by that (the tumour will be gone and you’ll move to the next stage of your treatment) and what you hear (you’ll be back to how you were before this started) may be two different things.
Communicating assertively
Mind your language – you might think that exaggerating can help others to understand the size and scale of what you’re dealing with but it does not help. It merely serves to stress both you and the individual that you are trying to talk to. Simple descriptions might be a bit boring and underwhelming, but they’re the way forward if you want someone to keep listening to you. Exaggerations and colourful descriptions can make other people feel overwhelmed and make them want to run away.
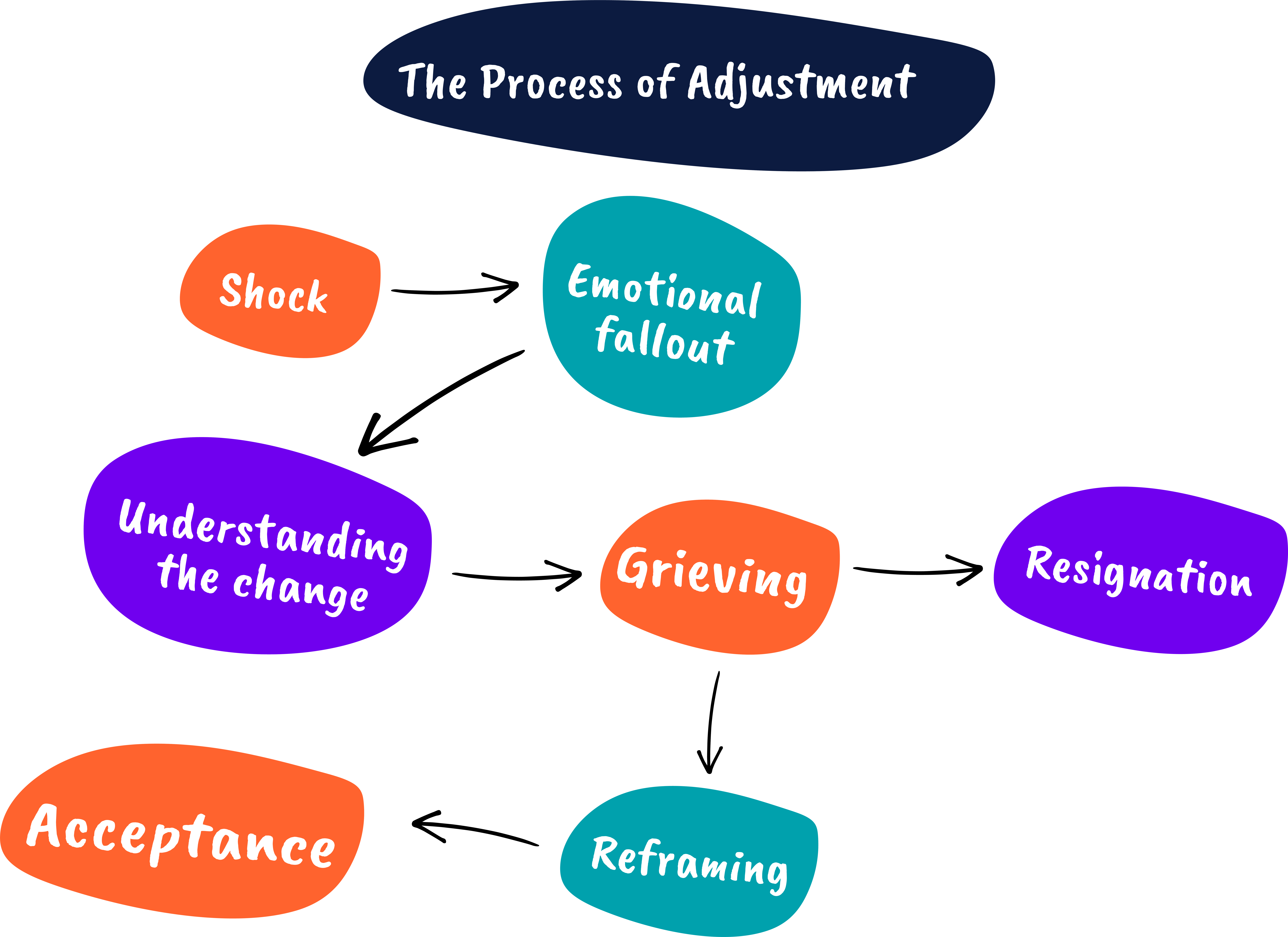
There are multiple different aspects involved in coming to terms with living with a chronic condition, including shock, various emotional reactions (including grieving) and various cognitive tasks such as understanding the change, until all those involved reach a point of understanding and acceptance.
As far as the content of the communication goes, it helps if you take responsibility for how you are feeling and are able to hear and accept that someone else may be feeling differently to you. There are multiple different aspects involved in coming to terms with living with a chronic condition, including shock, various emotional reactions (including grieving) and various cognitive tasks such as understanding the change, until all those involved reach a point of understanding and acceptance. Patients don’t experience their illnesses in a neat and tidy order and neither do their friends and family. So, you can be having a conversation about your condition trying to understand the changes involved, while they might be shocked, or having some other emotional reaction or struggling to comprehend the change that your condition is going to mean for your shared life together.
It’s OK to choose who you tell – not everyone reacts well to difficult or challenging situations. I have a friend who is lovely but whenever there is anything stressful or difficult that needs to be communicated it always ends up being about him and how he’s feeling. He means well, a lot of his reaction is because he gets stressed easily and he constantly worries about doing the wrong thing. But he’s obviously not the first person I’d be talking to about something where I need support. Indeed, he’s the kind of person where I would get one of our other friends to tell him our news, so I don’t have to deal with his emotional reaction. And no, that’s not cheating, it’s just sensible.
You need to accept that even having heard you, the other person may not be able to respond to your communication or meet your needs right now. They might need time to understand for themselves what it is you’ve told them. So, you might need several goes at communicating about your condition. That can be frustrating; it can feel like you’re doing it wrong, or that the other person isn’t interested, isn’t trying hard enough and doesn’t really care about you. The other problem with breaking up the conversation into small parts is that it can start to feel like it’s the only thing you ever talk about and that’s not good for relationships either. You need to be interested in what’s happening in the lives of the people in your life so your communications have some kind of balance. Additionally, we need to be able to be patient with each other and to forgive each other for the mistakes that are bound to be made along the way.
Sources of support
It’s not easy talking to others about having an unusual chronic condition – they may not understand or believe you and that can make you feel very alone. It’s normal to need to talk to others about what you’re experiencing but there can be lots of reasons why that feels too hard for your family and friends to deal with. You don’t have to be alone with it though. Remember that The Pituitary Foundation has both telephone buddies and a helpline you can call and they now have a new counselling service run by Rareminds. Additionally, The Pituitary Foundation has information about conditions that can help you to prepare to explain them to others at work, school or in doctor’s appointments.
Recording of Dr Jackson's presentation
One of my aims in life is to help people find words to describe what they’re experiencing and how they’re feeling. This blog post offers some, hopefully, useful words for those with pituitary conditions and their support networks along with some guidance on how to pronounce them for the trickier looking ones.
(Note on pronunciation – For the trickier words, I’ve broken them down into their various simpler sounds. You don’t pronounce the letters in brackets, they’re there to help you get the sound right. So, in the word inanition, below, where it says i(t) it’s telling you that you want the short ‘i’ sound from the word ‘it’.)
Inanition (Pronounced in-an- i(t)-shun): a lack of vigour, vitality, or enthusiasm due to a lack of nourishment be that social, physical, mental, or spiritual in nature. Inanition is a useful word to describe some of the limitations that living with a chronic health condition places on someone, as well as the impact of being a carer. If we take fatigue as an example (a commonly reported symptom of those with pituitary conditions as well as carers) it forces you to choose what you’re going to spend your energy on. People often report that they prioritise spending what little energy they have on work and home responsibilities, but this potentially leaves them with little or nothing left for socialising, hobbies or other meaningful activities and fun stuff thus leaving them starved of social contact, mental stimulation, and effective methods of relaxation and restoration. These various forms of starvation have an impact over and above the fatigue, and the ensuing lack of balance in our lives (you know what they say about all work and no play) leave people feeling flat with little or no enthusiasm and lacking interest in the world around them.
Immiseration (Pronounced (h)im-miz-err-ay-shun): defined by the Cambridge Dictionary as the act of making people (or a country or an organisation) poor. It’s unfortunately the case in this country that we no longer have a properly supportive welfare state. Coupled to which is an increasing tendency to blame people for getting ill and/or for not trying hard enough to get better. We’re all supposed to be dedicated to growing our country’s economy, but that isn’t matched by Government spending to improve life for the people who live here. Those with a pituitary condition aren’t to blame for getting their condition. It’s not uncommon for people with pituitary conditions to find that they need to change job because the long-term effects of their condition mean that they can no longer effectively do the job they were doing before, or they have to work reduced hours. Both of those can lead to reduction in income, and this can then mean having to move to a different part of town where the housing is less expensive. If you can’t afford to work then the current rates of financial support provided by the Government aren’t enough to enable even a basic standard of living, never mind a good quality of life. And since people with long-term conditions often incur extra expenses (such as paying for prescriptions, travelling to hospital appointments etc), having a chronic condition can very quickly push you into poverty. I like immiseration as a word because it acknowledges the misery that comes with not having enough resources to be able to live.
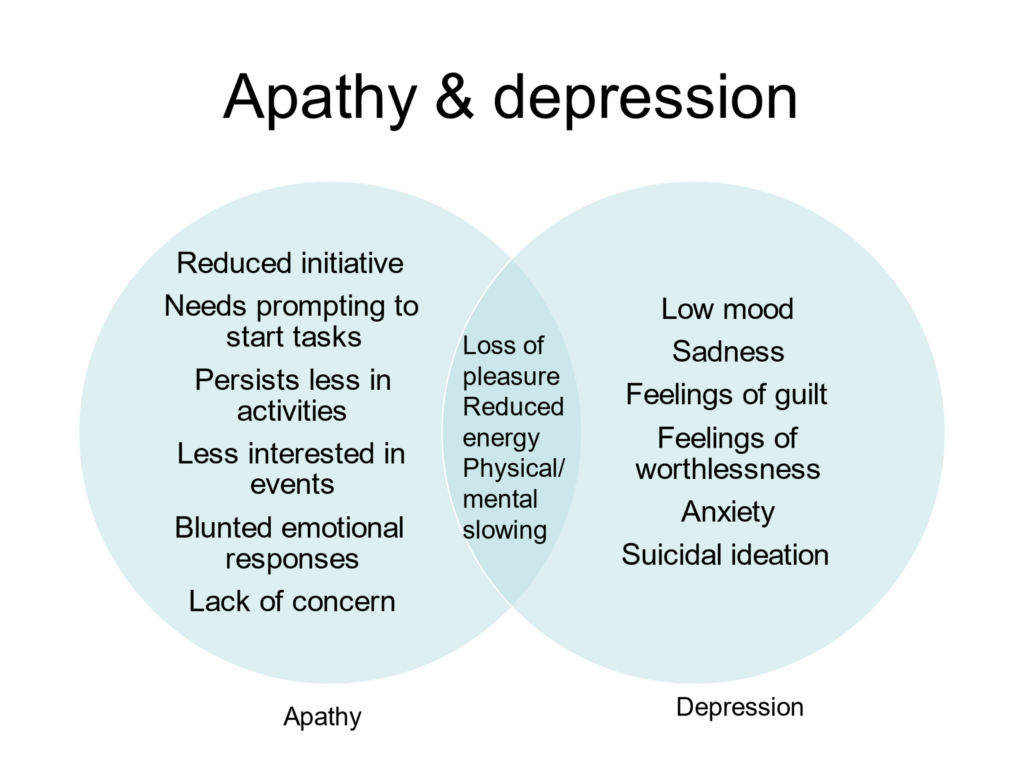
Apathy: a lack of interest, enthusiasm, or concern. You can have global apathy (i.e., no interest in anything at all, something that can be seen in people with some types of brain injury), or you can experience apathy in respect of one area of your life. For example, you might be so fed up at the way our politicians have been behaving, that you have no interest or enthusiasm for the upcoming elections. If you believe that your vote doesn’t count for anything, you might also think that it doesn’t really concern you either. There’s an interesting scientific paper from 2005 by Michael Weitzner, Steven Kanfer and Margaret Booth-Jones who described how their pituitary patients had apathy syndrome which they describe as a neurobiological illness, in other words, an illness caused by damage to the brain. Apathy is often misdiagnosed because its symptoms overlap considerably with those of depression (see drawing right). Based on anecdotal evidence, I’d say most people who describe a lack of interest, enthusiasm, or concern in respect to any or all aspects of their life are likely to be diagnosed with depression and offered anti-depressants.
Burnout: aphysical or mental collapse often caused by long term overwork or stress. It can also be described as the gradual erosion of a positive state of mind. Burnout is associated with an overwhelming feeling of emotional exhaustion of a sort that isn’t curable by resting. Burnt out people can often feel a sense of detachment, a feeling of dread or resentment at having to do things. Oddly to my mind, because it’s often caused by doing too much, it seems strange that burnout is often accompanied by a feeling of a lack of accomplishment. Burn out can lead to cognitive problems such as problems concentrating. I’ve included it here because it can occur in people with pituitary conditions who are valiantly trying to do all the things they would usually do in the face of their condition. It’s not a given that everyone with a pituitary condition faces problems in doing their usual activities, but some people are more affected by their condition than others. Our society these days puts great emphasis on the idea of working through or despite bouts of ill health. As a society we seem to be losing touch with the idea that resting is an important part of life, especially when we are not well. This societal pressure can cause people to push themselves to do things which can ultimately leave them so resource-depleted they burn out.
Ambiguous loss (pronounced: am-big-you-us): describes a loss that isn’t clear, usually the loss of a loved one. The person is alive, but they have changed so much that for themselves and for others they can seem like a different person. So, for example, a family member of someone with a pituitary condition might feel ambiguous loss if the person with the condition is different to how they used to be and it’s not clear if they’re ever going to return to how they were before the condition emerged. A person with a pituitary condition might experience ambiguous loss if they’re struggling to recognise themselves in how they’re respond to things. So, in essence, it’s something of a confusing state, where the person concerned is feeling that something is wrong, that a significant change has occurred, and it’s a change that leaves them feeling bereft in some way. Ambiguous loss goes to the heart of what it means to be human.
By Dr Sue Jackson
Sue is an Associate Lecturer at Plymouth University and an Independent chartered psychologist. She also works as a consultant for a variety of charities and pharmaceutical companies. Sue is a science writer and researcher working on a variety of projects round the UK.








